Neurotypical And Metabolic Disorder
I’ve held onto this story for a long time. The words have circled my mind over and over, yet I struggled to gather them in a way that honored both the truth and the tenderness of my heart. I worry my voice might sound angry — when really, beneath everything, I am simply grieving and deeply broken-hearted.
If anything here stirs anger or defensiveness, I gently invite you to sit with it for a moment. Often when we peel back that first layer, we uncover conviction, compassion, and even healing. My intention is not to shame or burden anyone, but to offer a glimpse into the world of a mama whose child suffered brain damage — and what that really meant for us.
Before I go further, I feel it’s important to explain what happened to Sterling. I debated sharing this part, because whether he was born with or without brain damage wouldn’t have changed the love we had for him, or the depth of our loss when he died. But this piece of his story matters — especially if it helps others understand Urea Cycle Disorders a little better.

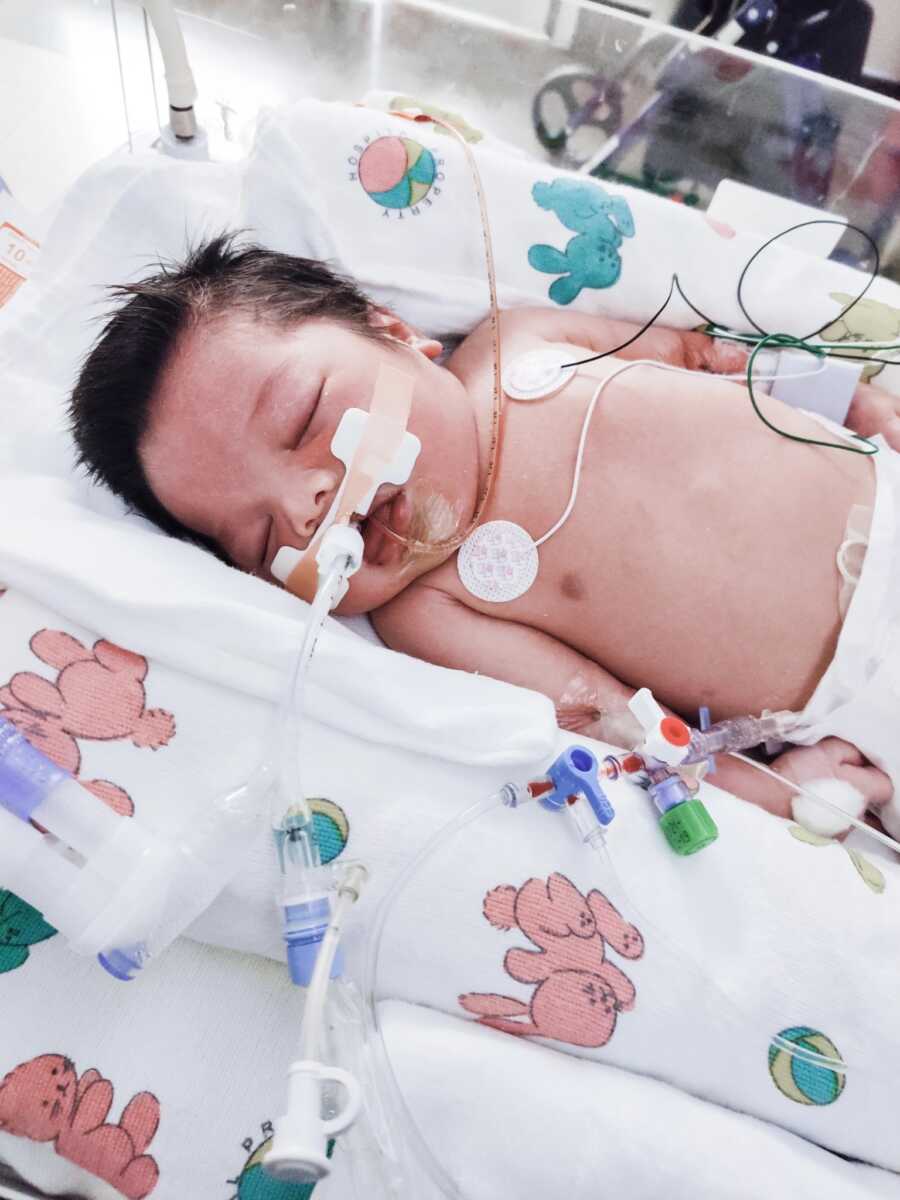
Sterling wasn’t born brain damaged. He entered the world as a healthy, neurotypical newborn. His injury wasn’t from lack of oxygen, HIE, or complications during birth. Instead, he was born with a rare inborn metabolic error. My husband and I were tested — we are not carriers. Doctors discovered it was a random mutation unique to Sterling. The condition, part of a group called urea cycle disorders, is known as Ornithine Transcarbamylase deficiency, or OTC.
OTC is a liver enzyme responsible for helping the body process protein and eliminate ammonia. Without it, ammonia builds up in the bloodstream — and ammonia is toxic to the brain. If high levels go untreated, the damage can become permanent and severe. The only hope is early diagnosis and immediate treatment, and outcomes vary widely. Two people with the same disorder may live entirely different lives depending on when and how they were treated.
So while Sterling was born neurotypical, his metabolic disorder silently worked against him. With every feeding, his tiny body couldn’t break down proteins properly. Ammonia filled his blood and, as days passed without a diagnosis, his brain soaked in those toxins. Eventually the damage was catastrophic. His brain shut down, and with it, all of his organs. And then he was gone.
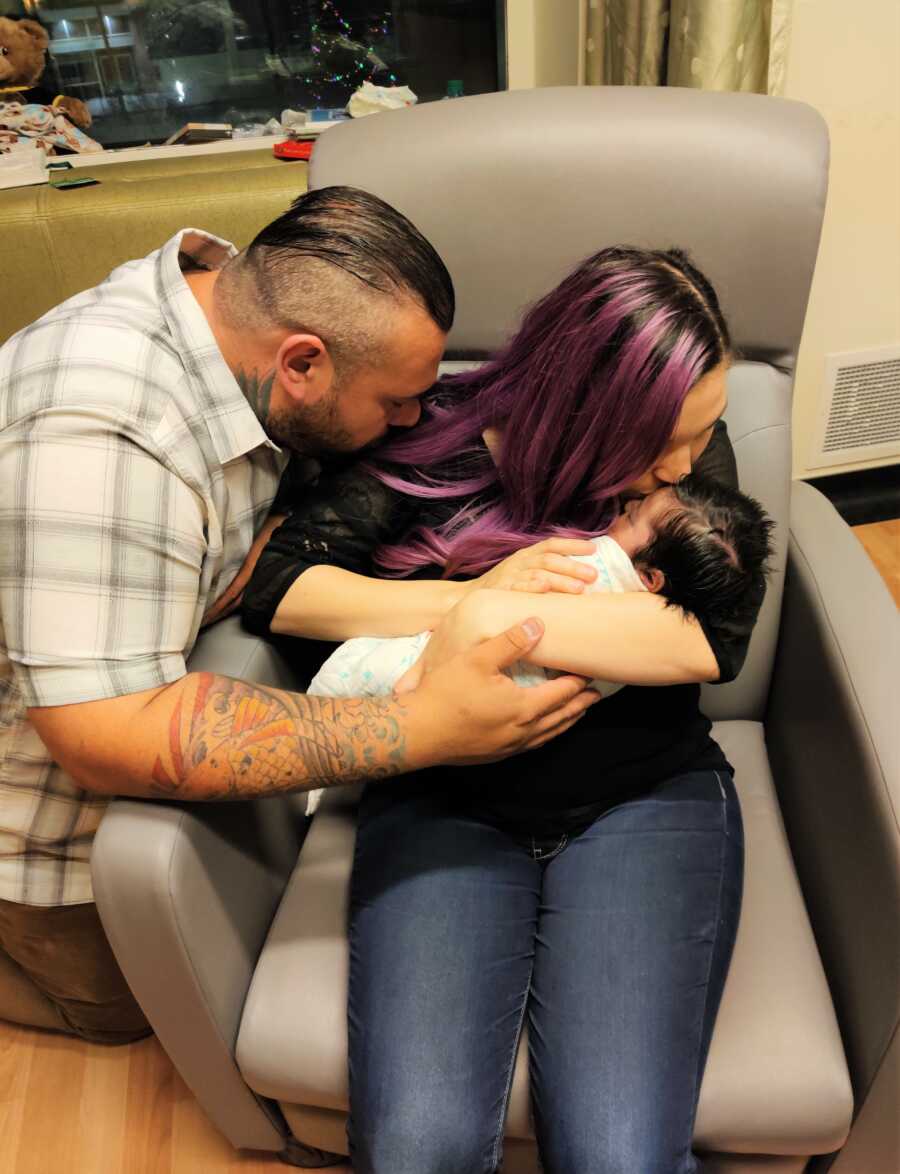
I still wonder sometimes — what if they had caught it? What would his life have looked like? There’s no real answer. Everything would have depended on timing, treatment, and how well his condition could have been managed.
People often ask about “quality of life.” Those words pierce me every time. At first, I hesitated to share that Sterling had suffered brain damage — not out of embarrassment, but because I know the world we live in. Too often, someone’s worth is weighed against their abilities.
When Sterling first died, people were devastated. They cried with us — until they learned about the brain damage. Then the tone shifted. Suddenly it felt as though the tragedy had softened in their eyes. Some even acted relieved, as if God had spared us from the burden of raising a disabled child.
I’ve heard words like:
“Think about his poor quality of life.”
“At least you won’t have to raise a brain-damaged child.”
“He would’ve been special needs.”
“He might have needed care forever.”
But here’s the truth: there is no universal measurement for “quality of life.” It is deeply personal. To assume someone is better off dead because their life might look different from ours is heartbreaking — and dangerous. If we really tried to rank lives like that, where would we stop? Chronic illness, depression, poverty, disability, trauma — would we say those lives matter less?
We don’t look at a starving orphan and say, “It’s better this way.” We don’t say it when addiction wins. Yet when someone with brain damage dies, people suddenly whisper that it’s “for the best.” Those words have never brought comfort.
Life is hard — for everyone — but that doesn’t give us the right to decide whose lives are worth living. We will never know what Sterling would have thought about his own life. That decision was never ours.
And then there are the words “at least.” Those two tiny words cut deeper than most people realize. They minimize grief. They gloss over suffering. And when they suggest that my child is better off gone, they wound me beyond measure. I would choose a brain‑damaged baby over a dead one every single day.
Sterling may have been disabled, medically fragile, or medically complex — and we would have loved him fiercely. We wanted him exactly as he was. I know I would have shown up for him with everything in me, and I would have needed others to show up with love instead of pity.

Even if caring for him had become a lifelong commitment, I would have chosen it without hesitation. The alternative — living the rest of my life grieving him — is far heavier than any caretaking ever could have been. When people act relieved that he isn’t here, it breaks me.
Having a child who suffered brain damage opened my eyes to how the world still views disabled people — as burdens instead of beloved souls. That stigma is painful, and we have a long road ahead in changing it.
I can’t say what Sterling’s life would’ve been like had he lived. I don’t know what challenges he would’ve faced. But I do know this: his life had value. He mattered as much as anyone else. He was cherished, wanted, and deeply loved. His story — different as it may be — was worth living. And so was he.