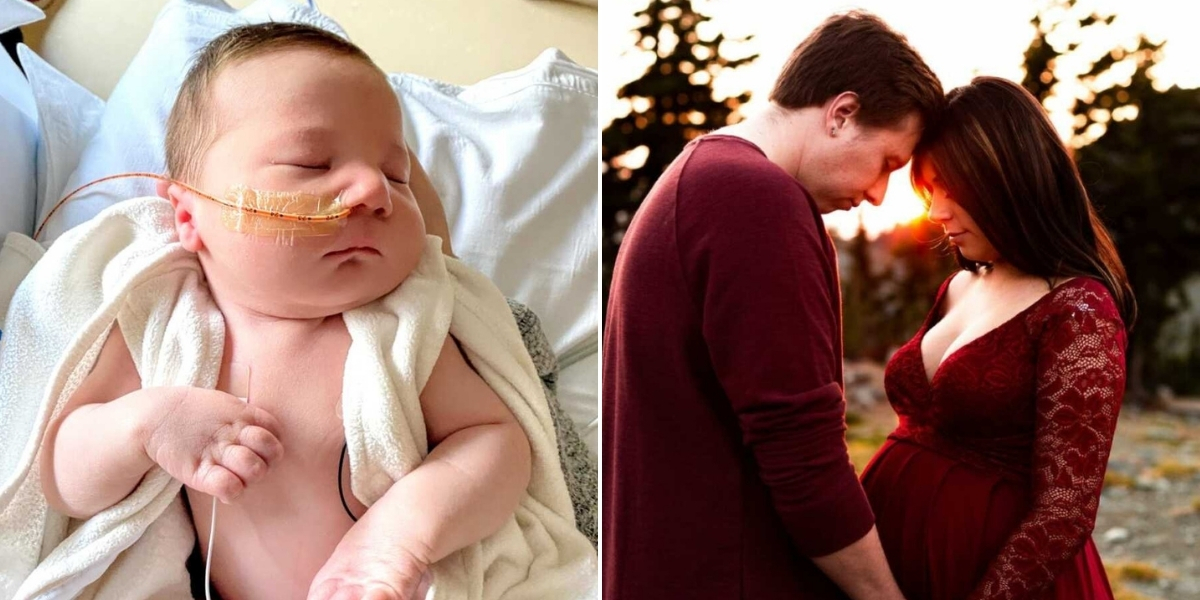
I found out I was pregnant in March 2020, the same week our state went into lockdown for Covid-19. I was 18, living with my aunt and uncle, and had only been with my boyfriend, Tyler, for three months. We were terrified—I was terrified. It took me two weeks to tell my family because I knew this wasn’t the “traditional” way to have a baby. When we finally told them, beyond the initial shock, everyone rallied around us. Their support, both emotional and practical, made a world of difference in those uncertain early days.
At our first ultrasound, we learned I was about six weeks along, with a due date of December 2, 2020. Seeing that tiny flicker on the screen, though, it didn’t quite feel real. That little wiggling circle would one day grow arms, legs, and a personality all its own. Because of the uncertainty surrounding Covid and pregnancy, I wasn’t able to return to work when the state reopened for essential workers. So, around 14 weeks, I started maternity leave.
The early months of my pregnancy were fairly easy. I had only mild nausea, occasional morning sickness, and some cravings. Because I was so young, doctors assumed there was little to worry about. At our 20-week ultrasound, Tyler and I were thrilled to discover the gender. After seeing our baby’s tiny face and nose on the screen, the tech finally said the words I had been waiting for: we were having a boy. Our sweet Theo. In that moment, it finally felt real, and my heart swelled with love I hadn’t even known was possible.
But as the tech continued measuring him, I noticed her repeatedly scanning his head and neck. I brushed it off, telling myself it was just first-time mom nerves. That night, I got a call from my midwife. The tone of her voice immediately set my heart racing. She said she wanted to see us first thing in the morning to discuss the ultrasound results. Tyler tried to calm me, saying it was standard procedure, but I couldn’t shake the feeling that something was wrong.
At the appointment, my fears were confirmed: “He has a thickened nuchal fold, a rocker-bottom foot, and we can’t see half his brain.” I sat on the patient table, staring at Tyler, barely hearing another word. Within days, we were at the nearest Maternal Fetal Medicine (MFM) office, over an hour away, for 3D ultrasounds and a consultation with a genetic counselor. The high-risk ultrasound tech was incredible—calm, reassuring, and even lighthearted—which helped normalize an overwhelming situation. The counselor later told us that, while Theo did have a thickened nuchal fold, his brain and feet were completely normal. We would still need an amniocentesis at a specialized hospital further south to confirm. For the first time, I felt a flicker of relief, clinging to the hope that maybe there was nothing seriously wrong.
Two weeks later, we had the amniocentesis. About a month after that, while trying to capture a video of Theo’s little kicks, I got the call that would change my life. The doctor’s words hit me like a freight train: Theo had a chromosome deletion that wasn’t documented in medical history. Children with similar deletions often experienced constant seizures, couldn’t eat, walk, talk, hear, or breathe independently, and might not survive birth. I sank to the floor, hysterical, cradling my belly, wishing I could somehow fix this. She said, almost casually, “Oh, you’re crying.” Of course I was crying! My baby’s life, my son, was hanging in the balance.
The next morning, we met with her again. She recommended we seriously consider our options, given that I was 28 weeks pregnant. She suggested a late-term termination as the best course, citing our age, my lack of a mother, and the difficulties of caring for a child with special needs. I had just turned 19, and I thought I should trust her guidance. But when we met the doctor at the MFM hospital—a calm, compassionate specialist in fetal genetics—everything changed. She congratulated us on the pregnancy first, then explained Theo’s deletion didn’t mean a death sentence. While it could affect his development, there was no certainty about what his future held. We decided to give Theo a chance, to see what he could teach us and what he could do.
The remainder of my pregnancy was physically typical but emotionally intense. I grew round, attended weekly prenatal appointments, had fetal echocardiograms monthly, and 3D ultrasounds every two weeks. At 37 weeks, our doctor told me I’d need to be induced by Monday at the latest, given the distance from the MFM hospital. Tyler and I carefully reviewed our birth plan and booked a hotel to wait for the call.

On Sunday at 4 p.m., we were called in. I was officially in labor by 9 p.m. It was slow, punctuated only by a few drops in our heart rates. I barely felt contractions until 7 cm and took only a Tylenol for pain. The epidural didn’t work, but I pushed through. By 9 a.m. Monday, I was fully dilated. The room was filled with dozens of specialists for Theo’s care. After 12 hours of labor and 40 minutes of pushing, Theo was born. They placed him on my chest for just 45 seconds before rushing him away for examination. Tyler went with him, while I delivered the placenta, my heart aching to hold my son.
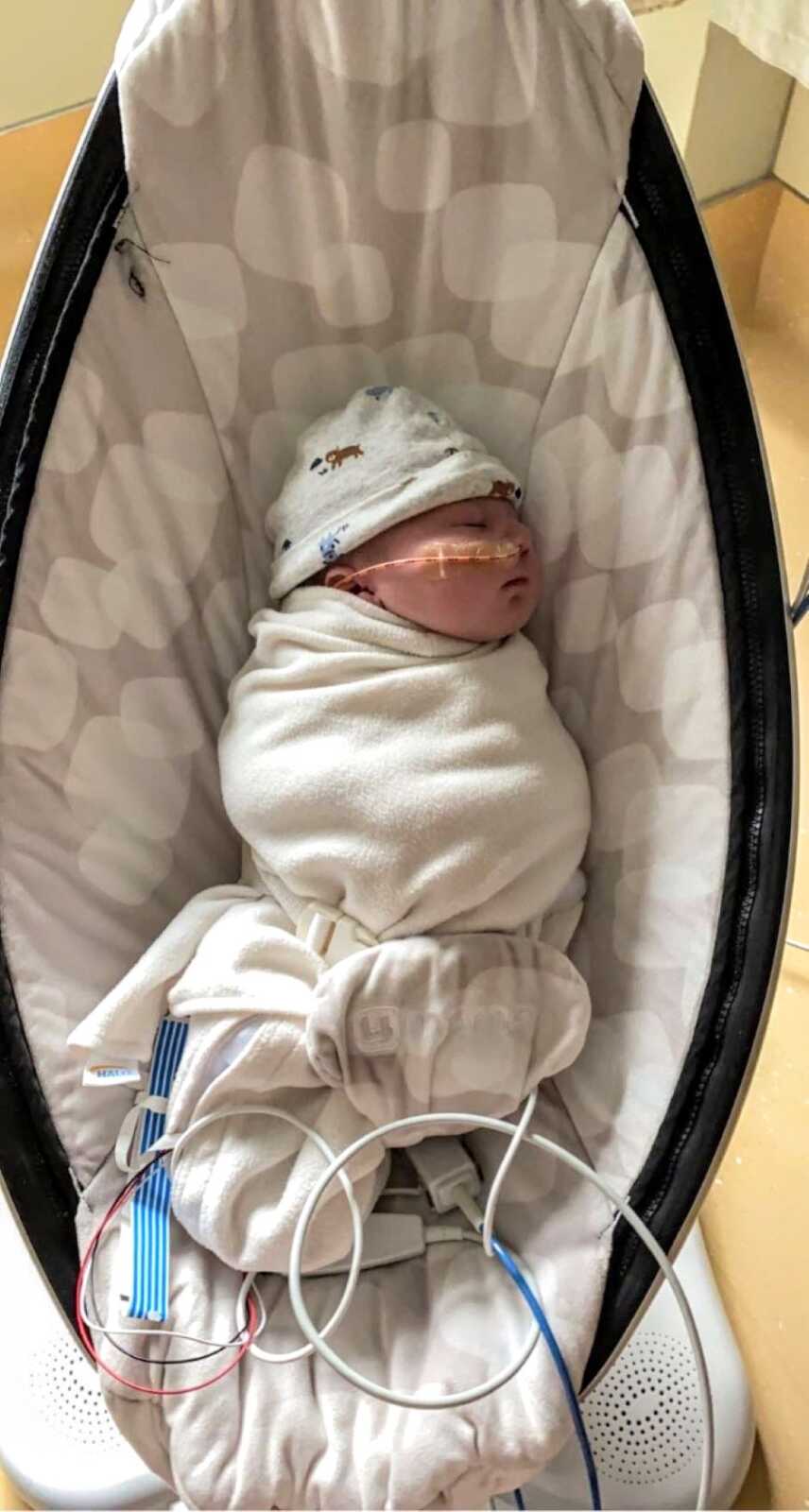
Theo spent 15 days in the NICU, facing breathing difficulties and congenital heart defects. Those days tested our faith, our sanity, and our relationship, but we left stronger as a family. He went home with a long list of therapies and specialists, and though we had a short period of “normal” parenting, challenges quickly returned.
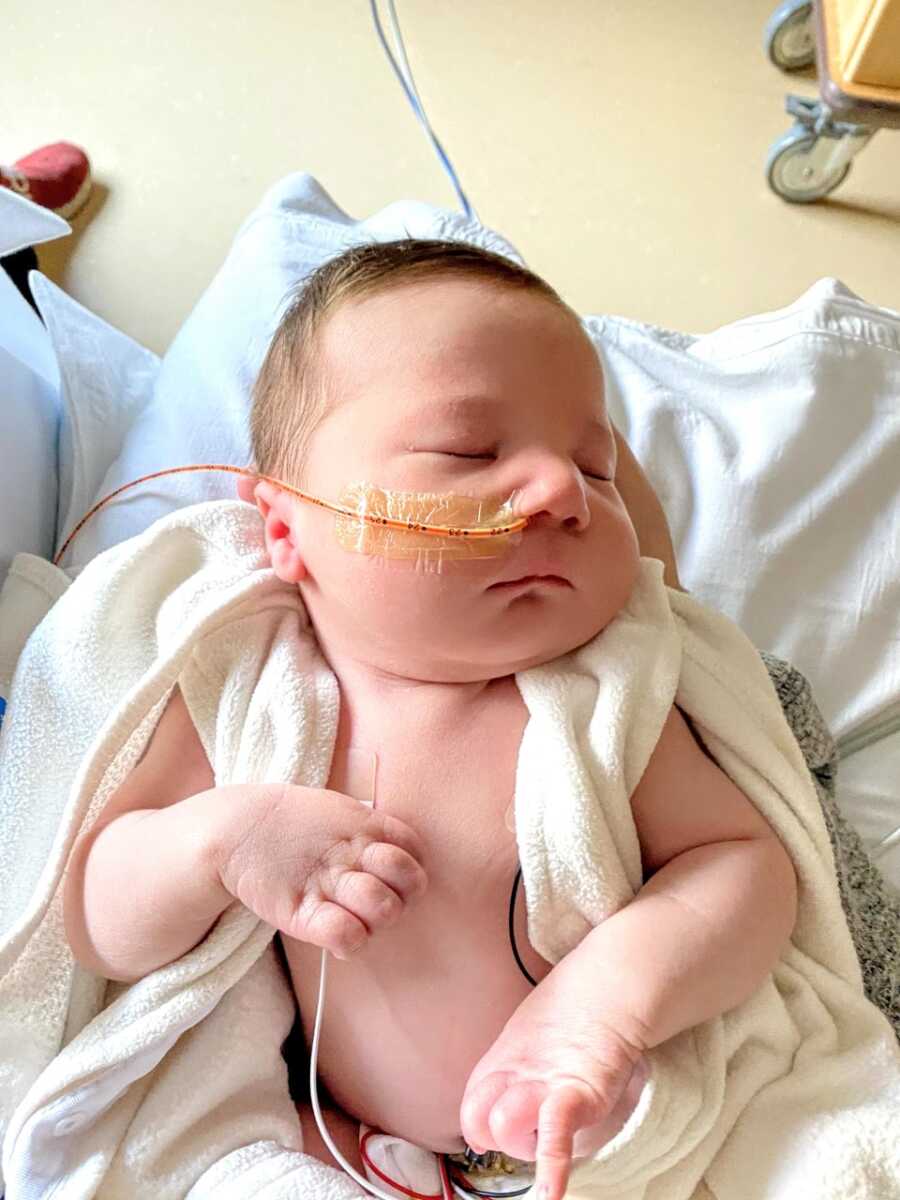
At three months, Theo stopped taking bottles and began vomiting constantly. On the way to the hospital, he choked in the car, and for a terrifying moment, we feared losing him. He was readmitted, required an NG tube, and later, at five months, nearly lost consciousness at dinner. Tests revealed dangerously low blood sugar, and subsequent hospitalization confirmed a severe viral infection. That 27-day hospital stay was exhausting, but we never left his side.
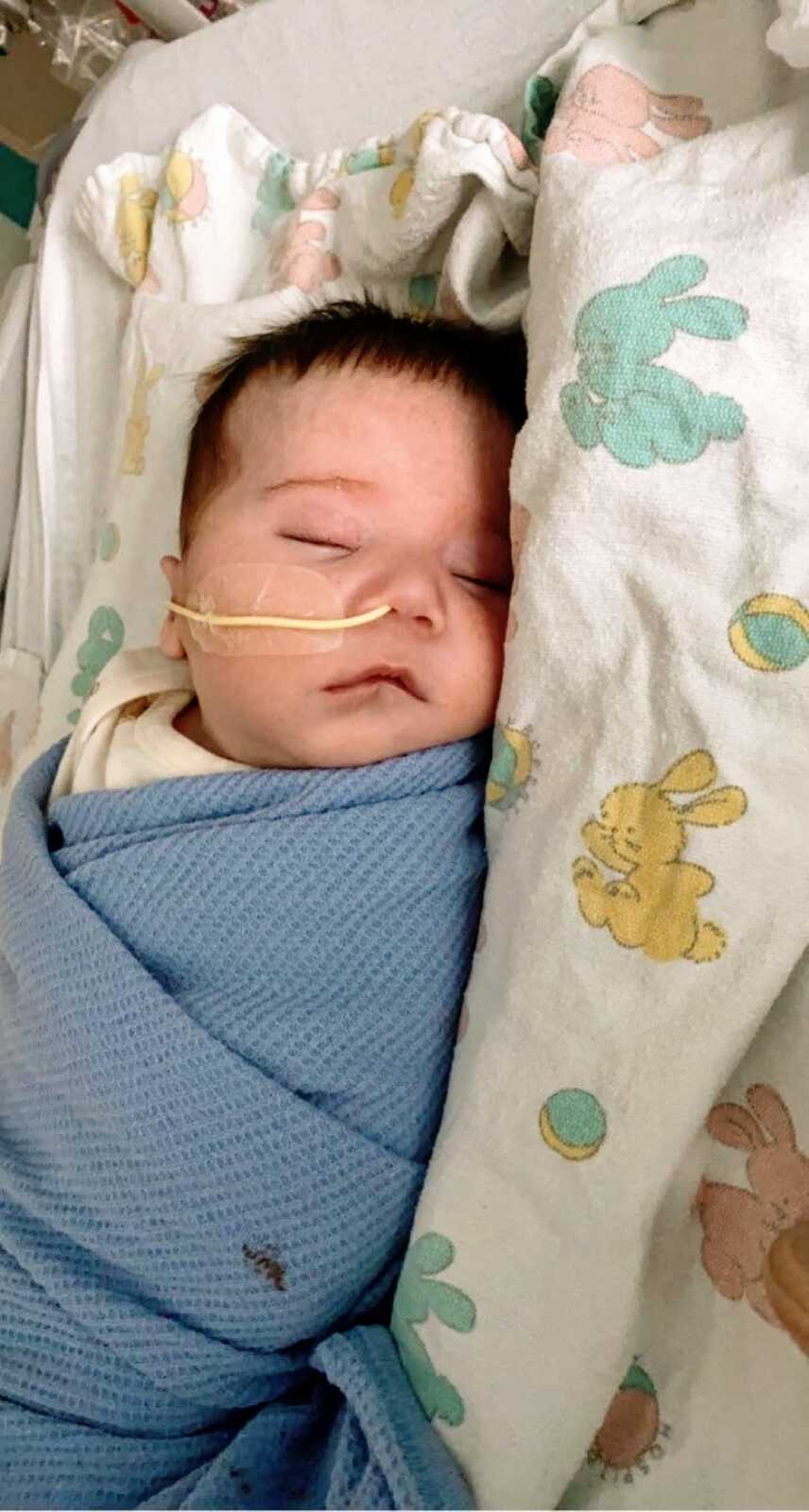

Theo will be one in three weeks. He has undergone two surgeries—a G-Tube placement and a hypospadias repair—and seen 13 specialties, now following ten. Unable to attend daycare, he stays home with me, attending multiple hospital appointments each week. Despite every obstacle, Theo is strong, joyful, and hilarious. Each day with him is a blessing, and we are endlessly grateful for the journey we share with our brave, beautiful boy.