From the time I was a little girl, I had always imagined myself as a mom. I dreamed of the chaos and love that would fill a home with children’s laughter. What I didn’t imagine, however, was how difficult it would be to get pregnant—or to stay pregnant. My husband and I met over ten years ago, and from the very moment after our first date, I knew he was the one. Four years later, we became husband and wife, sharing dreams of building a family together. Two children, we decided—two little hearts to call our own.
A year into our marriage, we felt ready to start our family. In September 2017, we naturally conceived, overwhelmed with joy. We immediately shared the news with our families and even bought a tiny onesie that read, “See you in April 2018.” That same month, we were also closing on our first home, excited to finally have a nursery ready. But just weeks after our positive pregnancy test, something felt off. I noticed some unusual discharge. It was a Sunday, and although I felt fine, my husband insisted I go to urgent care. Reluctantly, I went, telling them I feared a potential miscarriage. They told me they couldn’t help and directed me to the emergency room. That’s when the first wave of fear hit.

At the ER, I was assigned a bed and asked to change into a gown. Everything felt surreal and dramatic. The ultrasound showed everything looked normal for my gestational age, but they mentioned I had a heart-shaped uterus and advised me to follow up with my OB. The next morning, I called my doctor and was scheduled for an appointment the very next day. Naïve and hopeful, my husband and I went in, expecting reassurance. Instead, during the ultrasound, the technician asked, “Are you pregnant?” Confused, I reminded her that was why we were there. She backpedaled, saying the doctor would call later with the results.
That call came with a voicemail that left me anxious and confused. The embryo measured according to gestational age, but the heartbeat was not as definitive as expected. I was told to return the following week to “see which direction this would go.” Those seven days felt endless. When I returned for the follow-up ultrasound, I was optimistic—I had no symptoms of miscarriage. But the news was devastating: there was no heartbeat. We were given options: wait for nature to take its course, take medication, or schedule a procedure. I chose the procedure, and while it brought some closure, the grief lingered.

A few days later, I began passing clots and was told to return for a follow-up ultrasound. Not all tissue had been removed, meaning a second procedure was necessary. This time, my doctor could use a camera to investigate the heart-shaped uterus and discovered I had a uterine septum—a condition I had never heard of. I learned that I could have it surgically removed or keep it, but keeping it risked future miscarriages or preterm labor. Chromosomal testing showed the embryo was normal, but I also learned it had been a boy. That reality made the loss even more tangible, and I decided to have the septum surgically removed.

After meeting several fertility specialists, we found a doctor we trusted to perform the uterine septum resection. The surgery revealed that the septum was too large to remove in one procedure, so a second surgery two months later was required. It felt like a never-ending cycle of procedures—two D&Cs, two septum resections—but finally, everything was removed. Hope returned.

We tried conceiving naturally for months with no success, so we began IUI treatments. The first cycle ended in heartbreak. The second cycle, however, brought joy—a positive pregnancy test. Past experiences made me cautious, and I didn’t allow myself hope until we heard the heartbeat. But that hope was short-lived. Two weeks later, there was no heartbeat—another missed miscarriage. The grief hit harder this time, and I underwent another D&C. I became bitter, resentful, and envious of women who conceived easily. I channeled my energy into CrossFit and tried to occupy my mind, but the longing never faded.
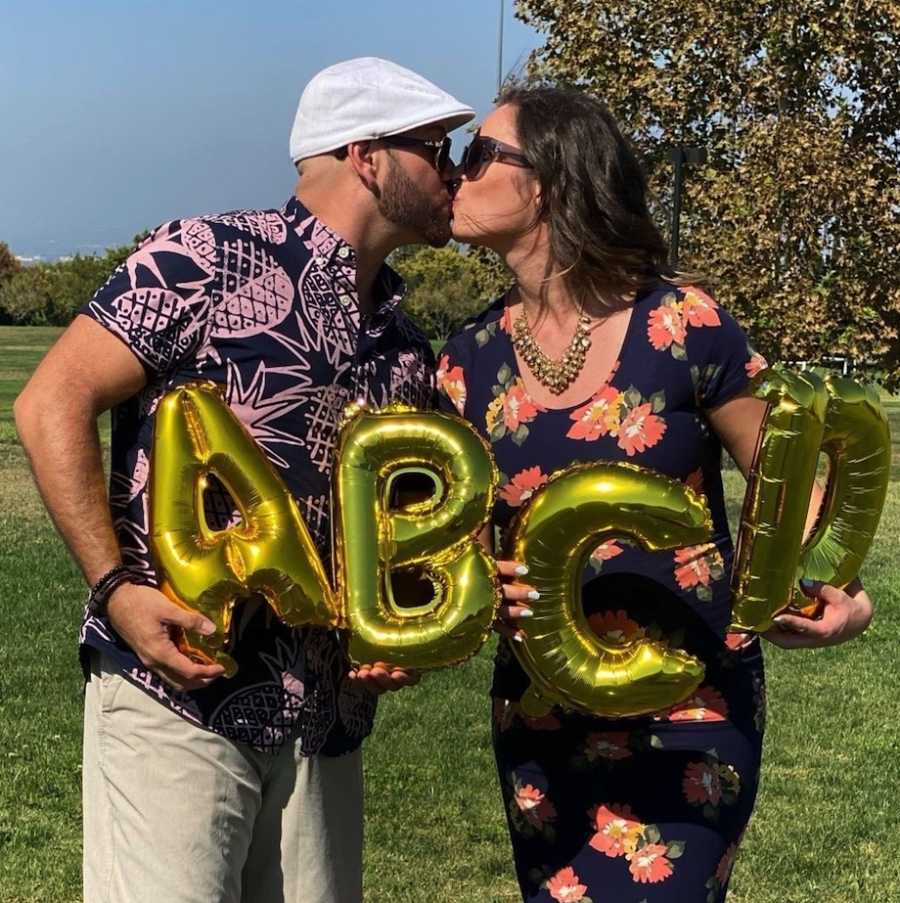
We continued with IUI cycles, faced setbacks, and even dealt with COVID-related delays. Injectable medications, multiple follicles, and several failed attempts tested my resilience. On what we hoped would be our final IUI, I nervously took a test three days early. Initially, I saw a faint line and doubted myself. The next day, the test confirmed it—two pink lines. I was pregnant, cautiously optimistic, until the 7-week appointment brought a terrifying sight: blood. My heart sank. But the ultrasound revealed something extraordinary: three heartbeats. Then a fourth. Quadruplets. Shock, laughter, tears—every emotion collided.


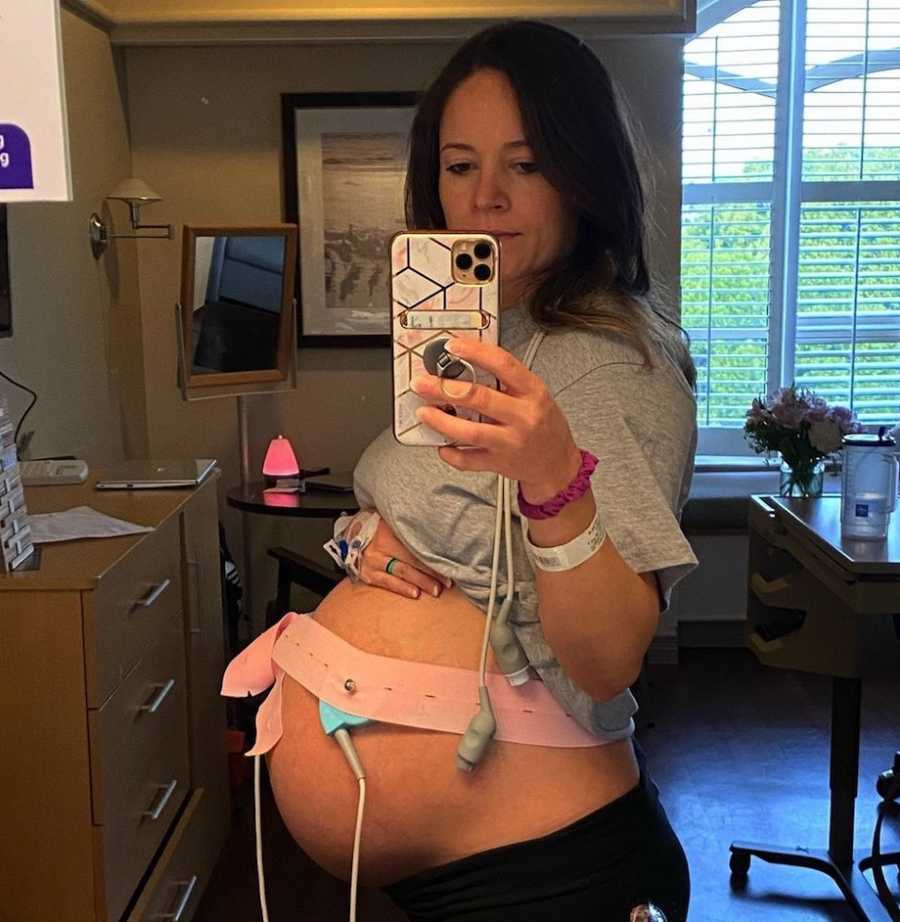
We were told it was a high-risk pregnancy, but we committed to carrying all four. Each week brought new anxieties and joys as we watched them grow. At 12 weeks, I transitioned to a perinatologist and was closely monitored. At 28 weeks, Baby C showed distress, and I was admitted to the hospital. Steroids were administered, and I was told delivery could happen at any moment. But our babies were resilient. At 31 weeks, they arrived healthy, spending a NICU stay of up to two months before coming home. They are now thriving at three months old—a miracle after years of heartbreak.

Through infertility, miscarriages, and medical procedures, I battled anger, jealousy, and despair. I hid my first miscarriage, felt alone, and struggled with negative thoughts. But sharing my story online and connecting with others revealed how common infertility is and how vital it is to lean on each other. If my journey can help even one person feel seen or less alone, then every moment of heartache was worth sharing.