“Mommy… am I going to get so sick that I die?”
Those words slipped from Charlie’s perfect little lips just days before his fourth birthday, and my heart shattered into a million pieces. The weight of his fear, so raw and innocent, left me trembling. All I could do was hold him close as tears ran freely down my face.
“I don’t want to have Cystic Fibrosis anymore. Can the doctors give me a pill to make it go away so I can feel better?” he asked.
Charlie noticed my tears and, in the purest act of love only a child can offer, wrapped his tiny arms tightly around my neck. “When I’m sad, snuggles always make me happy,” he whispered, “so I’ll snuggle you until your tears go away.” And so we lay there, two hearts comforting each other, clinging to the warmth we could offer. How I longed for his biggest worries to be scraped knees or sandwiches cut the wrong way, rather than a life-threatening illness.
I will never forget the first time I heard the words “Cystic Fibrosis” from a doctor. I’ve heard them countless times since, yet that first moment is etched permanently in my memory.
I had a routine pregnancy and a mostly uneventful birth at our local hospital in rural New South Wales. Charlie latched on to feed within the hour, and his first stool was black as the ace of spades—typical, the midwives reassured me. We returned home, lost in the wonder of our newborn, immersing ourselves in endless hours of gazing at this perfect little boy we had created.

It wasn’t until we received his Heel Prick Test results that a shadow appeared. During a check-up with our GP before his six-week immunizations, I was casually told that the test had picked up a common CF mutation. “Only one,” the doctor reassured me, “so probably nothing to worry about. Charlie’s growing well, putting on weight… but we’ll do a few more tests in Sydney just to be sure.”
Another Heel Prick Test followed, along with a Sweat Test. And then, after two excruciating weeks, the confirmation came: Charlie had Cystic Fibrosis.
CF is a relentless genetic disease, primarily affecting the lungs due to a malfunction in the exocrine system, which controls saliva, sweat, tears, and mucus. Lung failure is the leading cause of death. But what many don’t realize is that CF also attacks the digestive system—pancreas, liver, kidneys, and intestines. With over 2,000 possible mutations, symptoms and severity vary, and Charlie’s mutations were among the most severe.
The call from our doctor left me utterly broken. I sobbed for days, the bliss of new motherhood stolen with one phone call, replaced by uncertainty and fear. Even now, years later, the memory brings tears. Nothing has ever devastated me more than that night.
Though CF is genetic, no one in either of our families had it. The diagnosis was a bolt from the blue. Because Charlie hadn’t shown obvious signs, I clung to denial, convincing myself the tests must be wrong. The guilt of unknowingly passing on this gene consumed me. I spiraled into post-traumatic stress, ended up on antidepressants that made me feel numb, and would lie staring into space while Charlie fed hourly, Trav bringing him to the bed and back to his cot. It was during one of these feeds, as Charlie reached up to touch my face and smiled the brightest smile, that I realized I had to pull myself together. My fight was no longer for me—it was for him.

Fast forward four years, and Charlie is beginning to understand the harsh reality of his condition. He can connect sickness with the possibility of death. As a mother, every instinct tells me to shield him from pain, but CF doesn’t allow for that. It demands daily treatments, pills, physiotherapy, and vigilance. Charlie already takes up to 15 pills a day, with that number steadily increasing. There is no cure, no remission, no breaks. Every day is mentally and physically exhausting. Even the simplest activities—playing outside, visiting friends—require careful planning and risk assessment. Meals are calculated meticulously to match his medication. We monitor every sniffle, every cough, knowing that a minor illness can hit him like a ton of bricks, causing labored breathing, coughing fits, vomiting, and energy depletion. More physiotherapy, antibiotics, sometimes hospitalization… these are the rhythms of our lives.
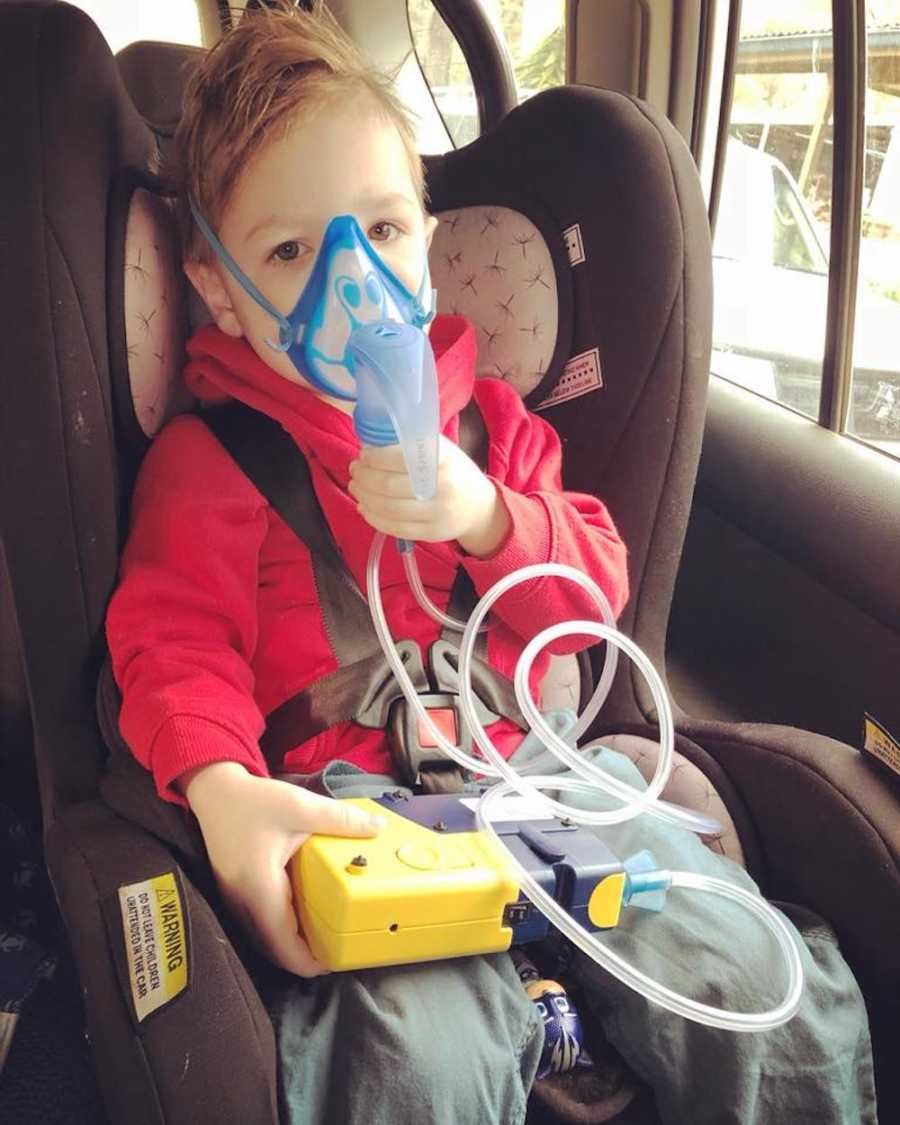
Charlie’s mutations are severe, meaning current breakthrough drugs available to 90% of the CF population won’t help him. Trials in the U.S. offer hope, but availability in Australia will take years. And even these drugs are not a cure—they merely attempt to slow lung deterioration while we wait for the day a real cure is found.

Despite everything, Charlie remains my light and my strength. I strive to give him a positive mindset and fierce determination to carry him through his darkest days. He radiates joy with a contagious smile, endless energy, and curiosity that amazes me. He greets strangers, shares stories of his favorite dinosaurs—T-Rex and Parasaurolophus—and absorbs knowledge like a sponge. CF has taught us to cherish the smallest moments, to find happiness in the everyday, and to celebrate every victory, no matter how small.
In just four short years, Charlie has endured more pokes, prods, tests, and doctor visits than most adults will ever see. Yet he carries on with grace, joy, and courage beyond his years. And every day, in his laughter and light, he reminds me why we fight so hard—for him, for the love he gives, and for the future he deserves.