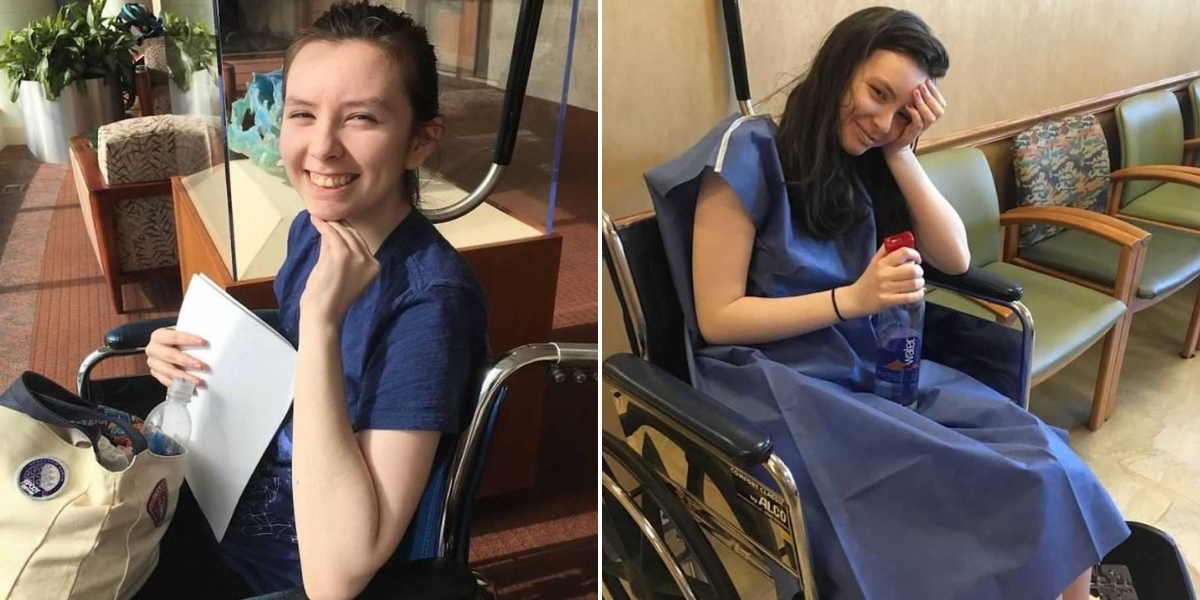
From birth, I was a healthy kid. Aside from the typical childhood illnesses—strep throat, ear infections, the usual—I rarely got sick. So when chronic illness hit me at age 11, it shocked everyone around me. One day in sixth grade, right after gym class, I felt suddenly nauseous, lightheaded, and noticed my heart racing. At first, I assumed I was just dehydrated and that the symptoms would pass. But hours turned into days, and days turned into weeks, and I realized something was seriously wrong. Even climbing the four flights of stairs at school left me so nauseous that I began to dread going. Yet, to those around me, it looked like anxiety. That’s how my school chose to treat it.
A few months later, I sat in the car with my mom, tears streaming down my face. She and my counselor had tried to get me into school, but I felt defeated. I was frustrated and angry that everyone insisted this was anxiety when I knew it wasn’t. I had been diagnosed with anxiety back in third grade, so I knew exactly how it felt—and this felt entirely different. That day, I kept telling my mom over and over, “This isn’t anxiety.” And so the cycle continued through the rest of sixth grade. With each passing day, my stamina dwindled, my body weakened from the constant effort of pushing through. But in August, a glimmer of hope appeared when I met with my doctor.

“I have an idea of what it could be, but I really hope it’s not,” she said, before mentioning POTS—Postural Orthostatic Tachycardia Syndrome—a type of autonomic dysfunction. Two months later, a tilt table test confirmed the diagnosis: my heart rate jumped 60 beats per minute every time I went from lying down to standing. Finally, I had a name for what was happening to me, and I followed my doctors’ recommendations carefully. But my health continued to decline. Despite the diagnosis, school administrators still treated my symptoms as though they were anxiety, dismissing POTS as something unimportant simply because they had never heard of it. We eventually had to involve my therapist to explain that my condition was medical, not mental.

By early 2015, I could only handle half-days at school; my body simply couldn’t manage more. My POTS doctor encouraged me to gradually return to full days, but each attempt made me sicker. Frustration mounted, and I felt like I wasn’t doing enough. Finally, in May 2015, I entered a pain and rehabilitation program, nervous but hopeful, following doctors’ recommendations. The first day went okay, mostly tests and program orientation. The second day, however, was harder.

After a full morning of activities, I felt ill and asked to see my mom. Parents attended alongside their children, so I knew she was nearby. But my request was denied because I was supposed to be in a group session. I felt sick and anxious, unwilling to go to class without her. I ended up sitting outside the entrance, crying, watching my mom through the glass. For an hour, I asked repeatedly to see her, but staff continued to refuse. Eventually, they brought my mom aside, suggesting that I might cooperate more if she went upstairs with me.

My mom, having lived in this town for over 20 years, realized that the program’s upper floor was actually a psychiatric hospital. The moment she understood, she took me and we left. We never returned. For the rest of that school year, I continued to attend school nearly every day, pushing myself to appear “fine,” fearful of another program experience. By summer 2015, I was able to go on a family vacation to St. Louis and visit relatives in Chicago. But by the beginning of eighth grade, the toll of pretending caught up with me. I had to leave school on the second day—barely making it through the first. I couldn’t even get out of the car the next day. Online schooling became my only option, but it came at a cost: I lost nearly all of my friends and plunged into isolation.

By August 2016, my stomach issues worsened; some days I couldn’t eat at all. I began losing weight, and simple movements caused pain and nausea. I stopped leaving the house entirely. By May 2017, I saw a gastroenterologist who referred me to a pain doctor. He recommended steroid injections into my abdominal wall, which I began receiving regularly over the next year, desperate for relief. Despite every intervention—POTS treatments, steroid injections, lidocaine patches, chiropractors—I kept declining. Leaving the house was exhausting, even for short errands or walking my dog. Eventually, I felt defeated. I had tried everything.
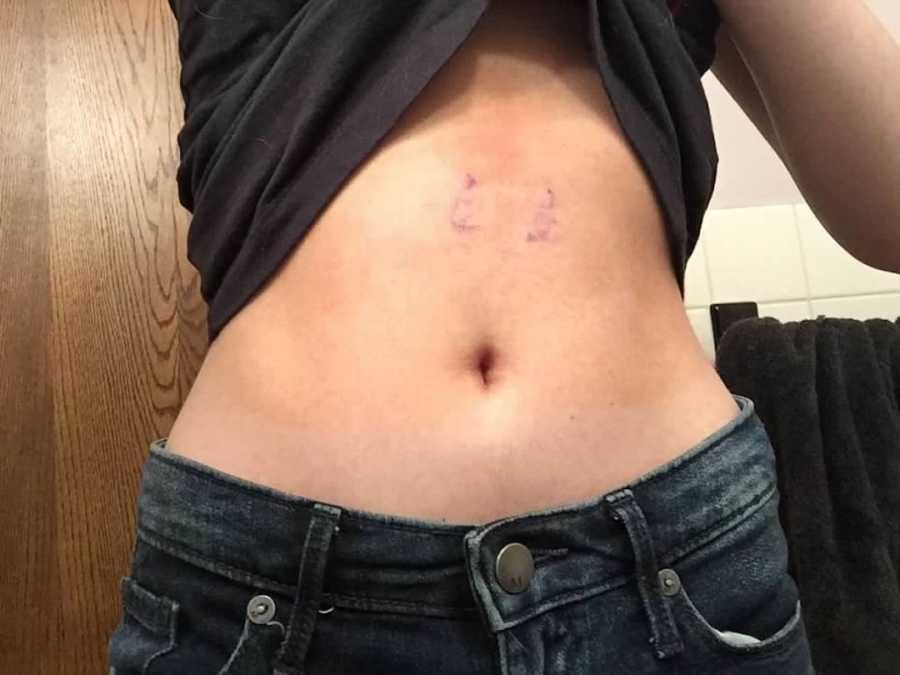
December 2018 marked my breaking point. My mental health deteriorated; with my therapist moving away and my doctor retiring, I fell into a deep depression. Panic attacks consumed my nights, and I cried so much my face ached. I felt completely alone until I turned to the internet. Searching for POTS on YouTube, I found videos of others living with the condition. Watching them, I felt less isolated. Many also mentioned Ehlers-Danlos Syndrome (EDS), a term I had never heard before. Intrigued, I researched it, and slowly began to see the connection: my hypermobility, joint pain, unexplained bruising, and POTS symptoms aligned with EDS.
By May 2019, I decided it was time to pursue a diagnosis. I saw multiple specialists—allergist, neurologist, gastroenterologist, and rheumatologist—but most dismissed me. My allergist minimized my symptoms, the neurologist sent me to therapy, my gastroenterologist blamed my pain on a pain disorder, and my rheumatologist did the same. When I mentioned EDS, he told me, “Even if you do have it, a diagnosis wouldn’t be worth it because you can’t do anything about it.”

Instead of giving up, I fought harder. In October 2019, a pain doctor referred me to physical therapy. I found a therapist experienced with POTS who explained the science of chronic pain more clearly than anyone had before. Meanwhile, I pursued genetics testing for EDS. My genetics appointment on February 6, 2020, changed everything. Though my doctor was initially replaced, he quickly recognized the signs: hypermobility, skin extensibility, and my medical history. He diagnosed me with Hypermobile Ehlers-Danlos Syndrome, saying, “I knew from the second I shook your hand.”
Relief washed over me. For the first time, I had answers. Everything made sense: the ACE bandages I wrapped around my ankles, the POTS, unusual bruising, dental crowding, and long fingers. Soon after, my grandmother was also diagnosed with Hypermobile EDS, making the discovery even more meaningful. I wasn’t looking for a cure—this diagnosis gave me clarity and the chance to protect my body moving forward.
To anyone still seeking answers: trust your body. Pain disorders are real, and your symptoms are valid. I spent years doubting myself because doctors dismissed me repeatedly. Know that you know your body best. Listen to it, advocate for yourself, and never let anyone else’s words make you question the truth your body is telling you.