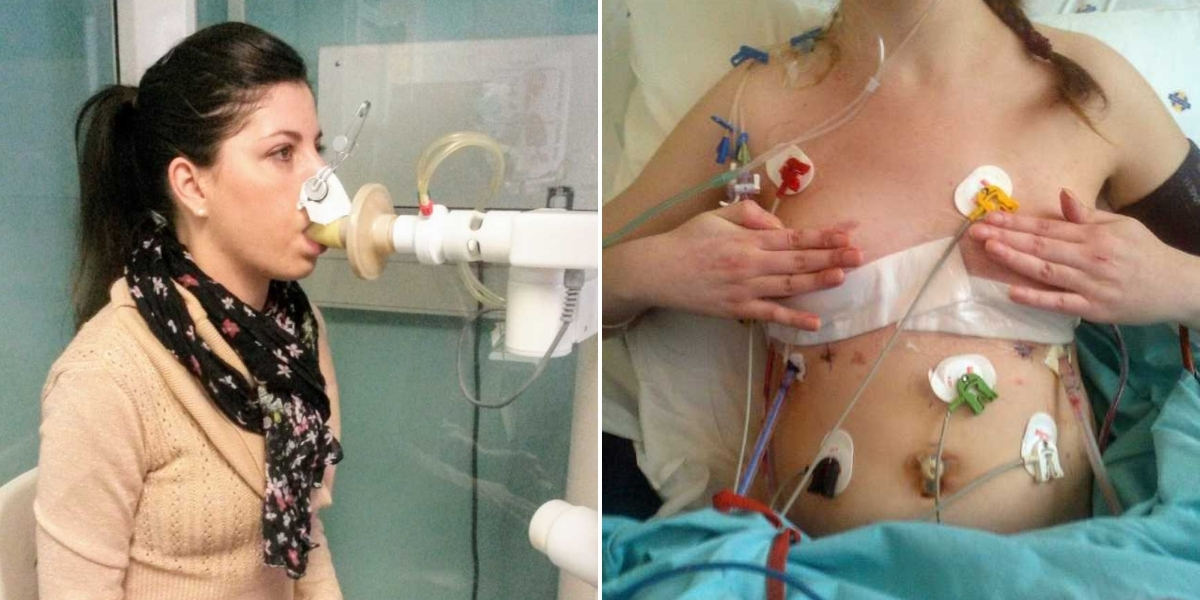
I was born in 1987 with a genetic disease called cystic fibrosis (CF). Back then, it wasn’t a well-known condition, and my parents spent countless months consulting different doctors, searching for answers. Finally, when I was a year old, they received the diagnosis. There was relief in finally having a name for what was wrong with me, but that relief quickly gave way to the daunting reality: the long, never-ending journey of keeping me alive had begun.
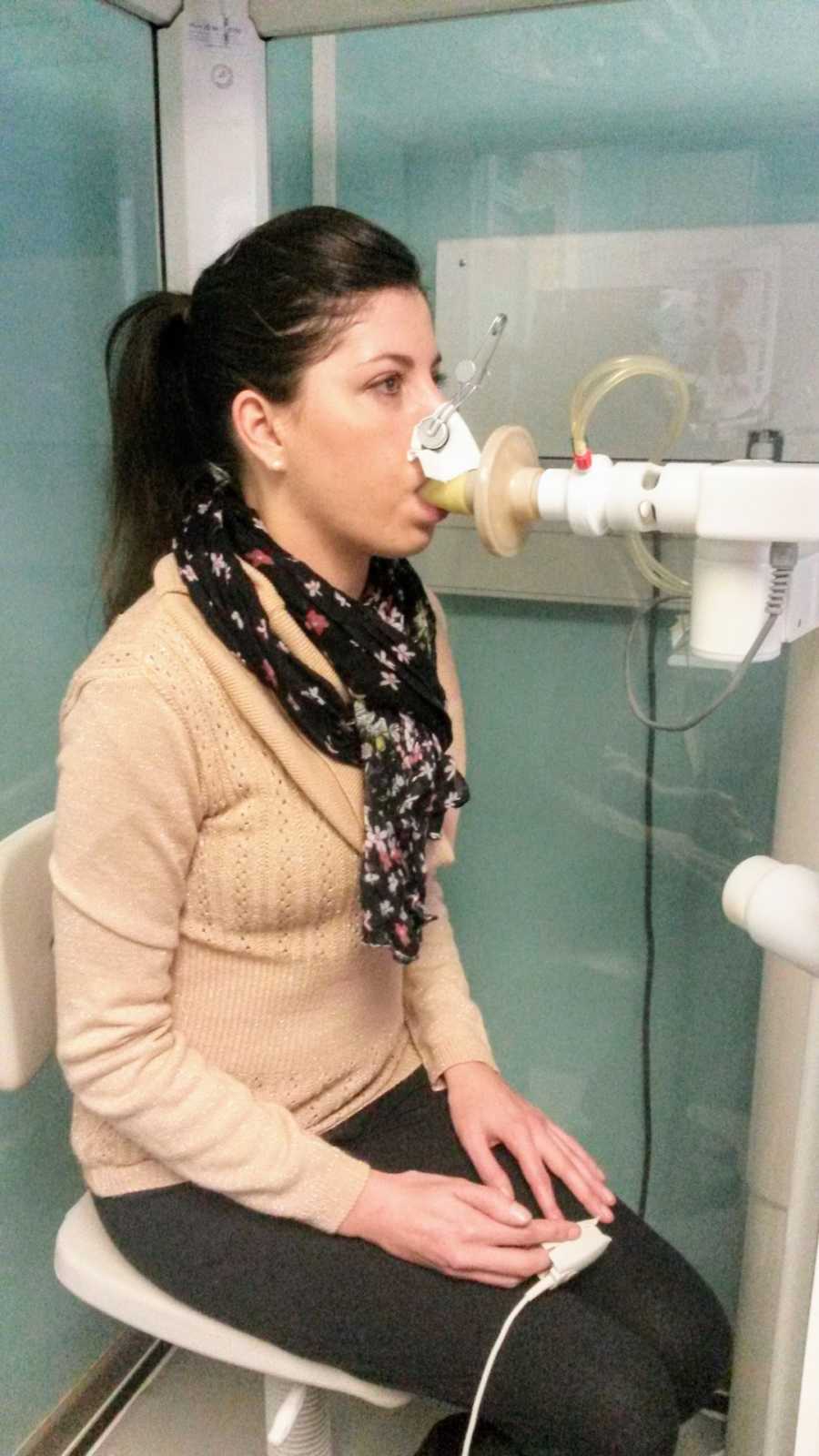
We lived on a farm in Zimbabwe, and I was the only known CF patient in the country. This meant regular flights to South Africa for treatments and medications that were literally keeping me alive. CF affects many organs, but the lungs are usually the most severely impacted, so pulmonary care started as early as possible. For me, this meant twice-daily nebulizing sessions to open my airways and help me breathe. Around the age of eleven, intravenous antibiotics became necessary to combat persistent lung infections, leading to two-week hospital stays every three months. I missed countless school days and normal childhood experiences—camping trips, parties, and afternoons with friends—due to infections that seemed to arrive at the worst possible times. To minimize disruption, I began doing IV treatments as an outpatient, going to school with a needle in my arm, wrapped securely, only missing afternoon activities while my medications were administered.
From a young age, I was empowered to manage my own treatments. During hospital stays, I handled my medications almost entirely by myself, relying on nurses only for supplies. Being so visibly different and constantly fielding questions from peers, teachers, and strangers might have been daunting for some children—but I felt surprisingly confident. My parents had instilled in me the belief that being different made me special, and that confidence has stayed with me throughout my life.
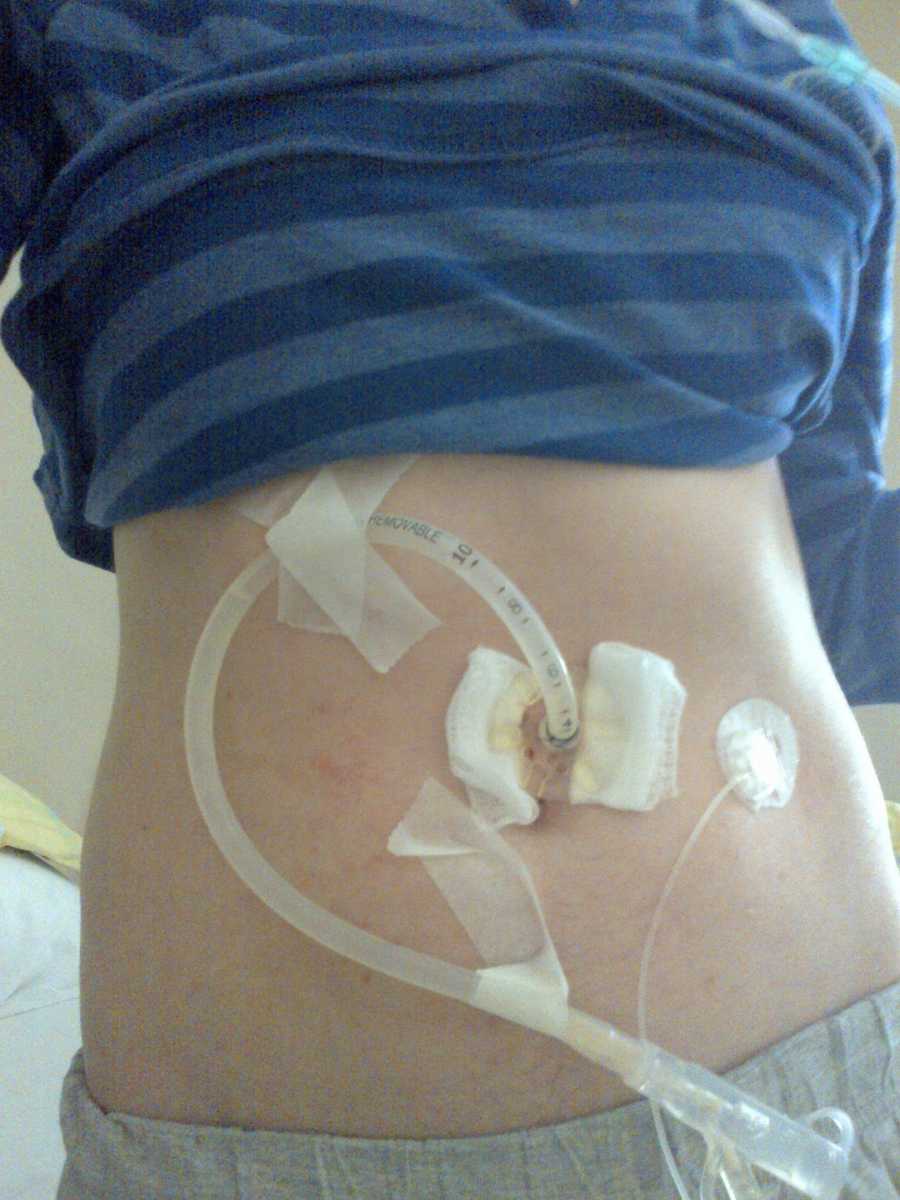
CF also impacts the pancreas, meaning I required artificial enzymes every time I ate to absorb nutrients. Weight gain was nearly impossible, and though being “skinny” might sound appealing, it brought its own challenges. I had to be force-fed protein shakes and high-calorie foods throughout the day, and eventually, I needed a permanent stomach tube—a PEG—to provide overnight feeding while I ate as much as possible during the day. My pancreas eventually failed enough to cause diabetes, requiring insulin with every meal. This created a complex balancing act: I needed to eat enough to maintain weight, but had to manage carbohydrates carefully to control blood sugar, all while adjusting enzyme doses. Every meal became a calculation, and I’ve never known the freedom of eating without planning medication or insulin.
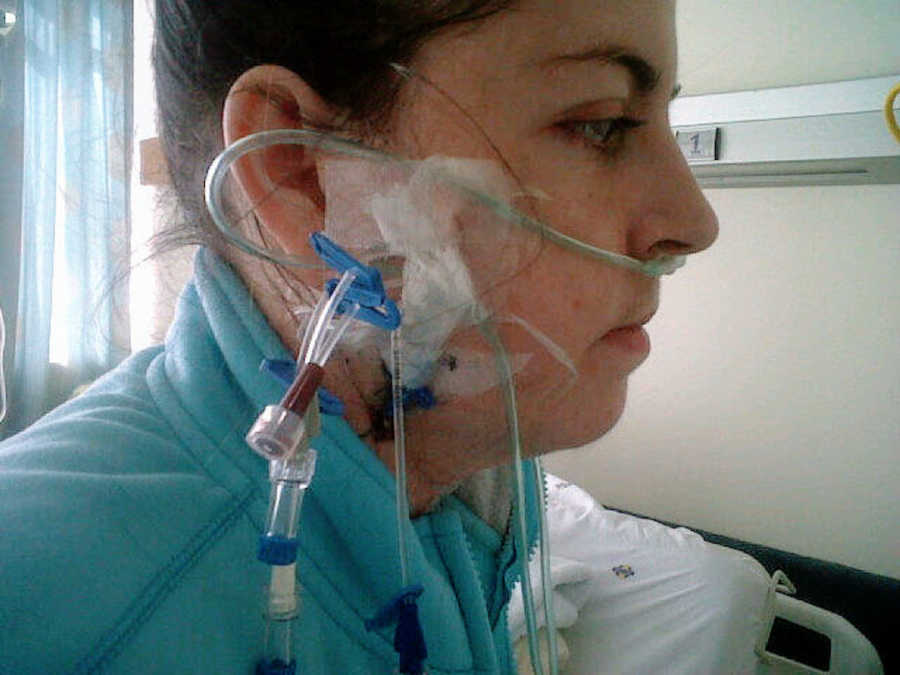
CF took a toll on my body in ways that went beyond medications. I couldn’t participate in sports; breathing became difficult long before my peers even broke a sweat. As my lungs deteriorated, each breath felt like a battle, muscles spasming around my chest as I forced air into failing lungs. I eventually needed 24/7 oxygen to survive. Even removing it for a minute—just to wash my face—left me blue, faint, and desperate for air.
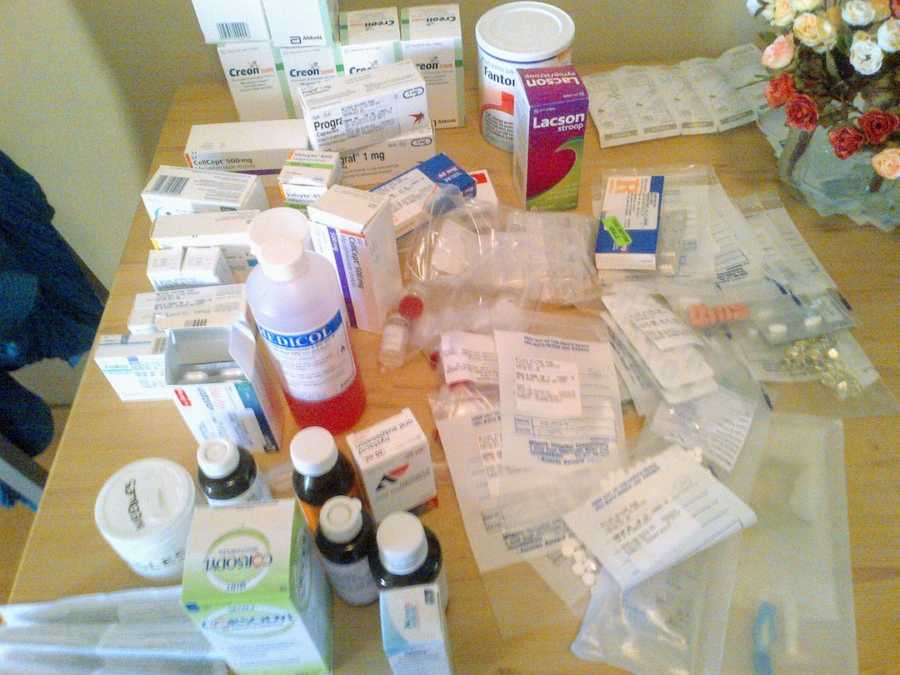
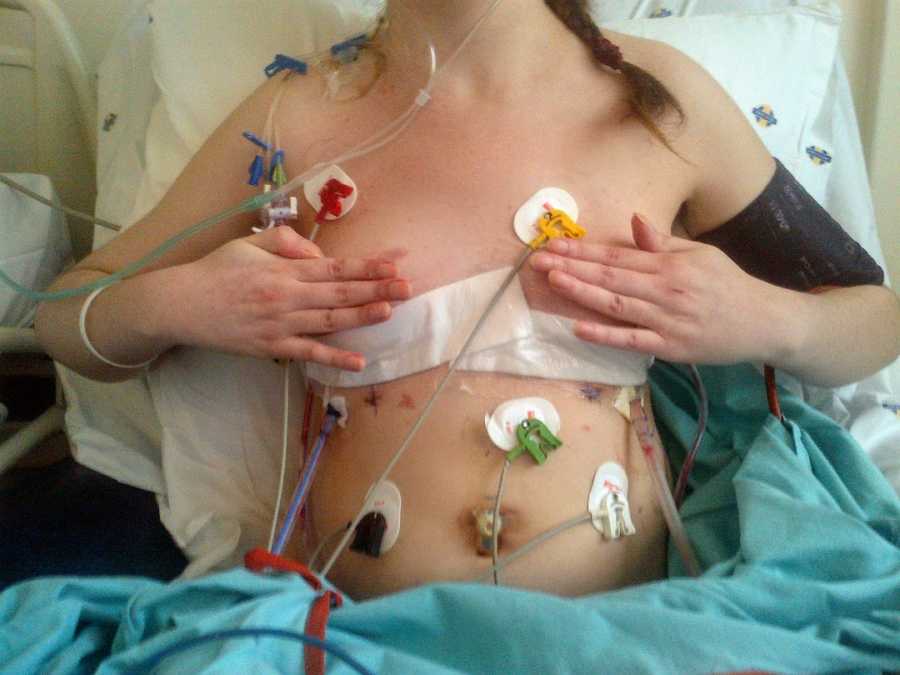
At 24, I was listed for a double lung transplant. My veins had been worn out from years of IVs, so a portacath was surgically inserted under my skin to allow easier access to my main veins. I also required an insulin pump to manage overnight tube feeding. My body was covered in tubes, each one vital to keeping me alive, and maintaining them was a full-time job. By this stage, I had moved to South Africa permanently to stay close to the transplant center. My incredible mom moved with me and cared for me every day while I awaited new lungs, completely bedridden, coughing through infections, leaving our apartment only for doctor visits or hospital stays.
Watching friends finish university, get engaged, or travel the world while I lay in bed was heartbreaking. Yet when faced with a 50% survival chance for a lung transplant, hope was motivation enough. During hospital stays, I bonded with other CF patients, sharing poker nights with bottle caps as chips. These friendships, though constrained by masks and distance due to contagious infections, gave me companionship and hope. Many of these friends didn’t survive, leaving me to navigate not only the physical challenges of CF but also profound grief.
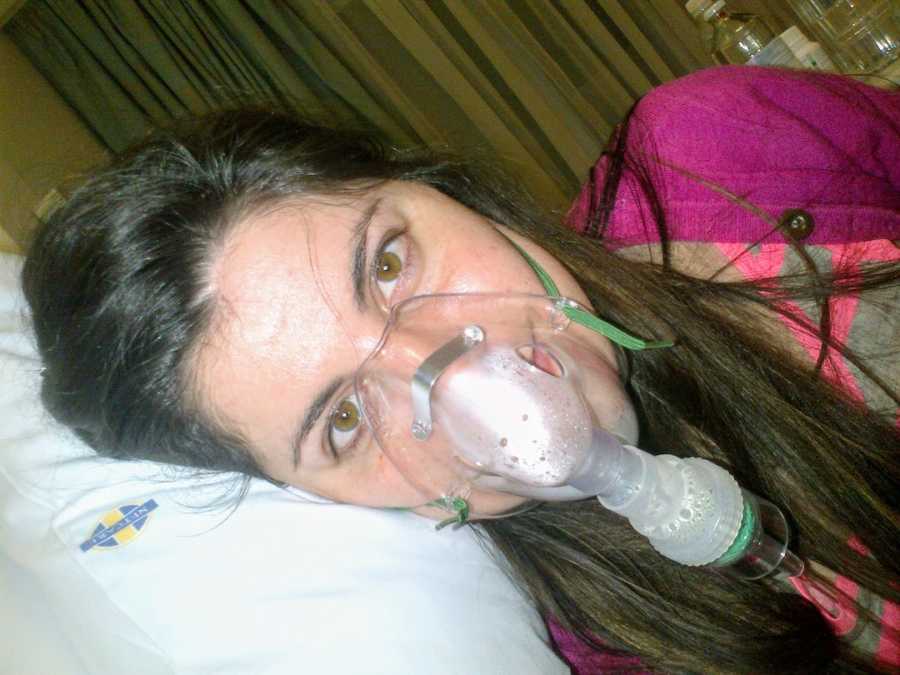
Finally, my moment arrived. During a hospital stay, my doctor informed me that a donor had been found. My mom and younger brother rushed to the hospital, my dad flew in from Zimbabwe but unfortunately missed the surgery, and family friends were there to support us. The eight-hour transplant began, and when I awoke, I was in ICU in a glass room with no visitors allowed for five days. Seeing my mom and dad waving from the other side of the glass was overwhelming—I could finally breathe without oxygen tubes.
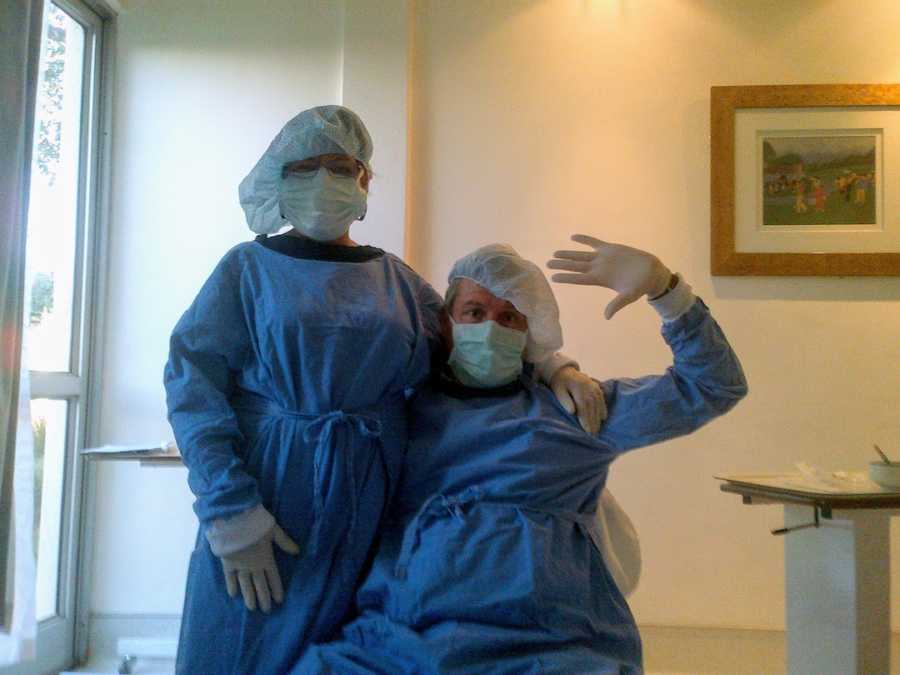
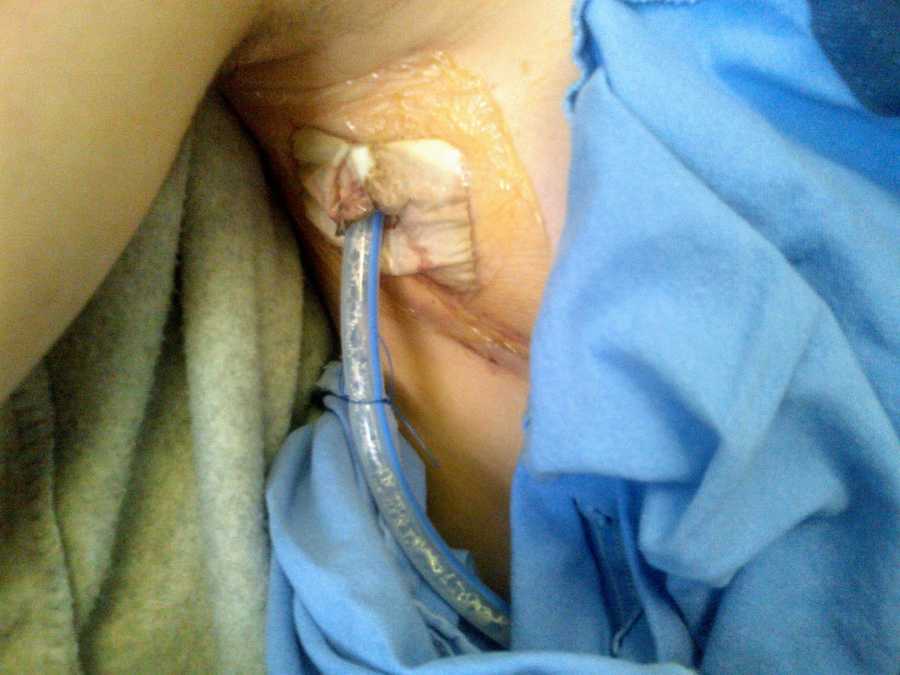
Recovery was challenging. My lungs initially functioned, but fluid buildup required pleural taps. The third procedure went wrong, puncturing both new lungs. I was rushed back onto oxygen, and large chest tubes had to be inserted, some becoming infected, leading to another ICU stay. My surgeon performed an experimental procedure using my own blood to clot the holes in my lungs—a lifesaving success. Three months after my transplant, I returned home.
Life with new lungs felt like being released from a zoo into the wild. I had no university education, few friends, and little confidence. Slowly, I found my footing—blogging, doing odd jobs, helping agencies with social media, then building my own company. I co-founded TELL (Transplant Education for Living Legacies), a charity raising awareness about organ donation. I met Travis through mutual friends, and we fell in love, marrying in a small, COVID-safe ceremony in 2020.

March marked my eighth year with new lungs, which continue to function beautifully. I manage enzymes, insulin, and anti-rejection medication daily, but I am free from oxygen, nebulizers, and lung rehab. Biokinetics helps me maintain strength after years of severe lung weakness. Life before and after transplant feels like two separate worlds, yet the journey didn’t end there. Shortly after my recovery, my mom was diagnosed with stage-four breast cancer and passed away three years later. Around the same time, my aunt and uncle, who had cared for me in South Africa, died in a helicopter accident. Political instability in Zimbabwe led to our farm being stolen, forcing my family to rebuild from nothing.

Through it all, I am deeply grateful to my donor for giving me a second chance. Every day is a gift, a reminder of resilience, love, and the relentless fight for life. I have survived unimaginable challenges and continue to embrace life fully, celebrating each breath and every moment I am alive.