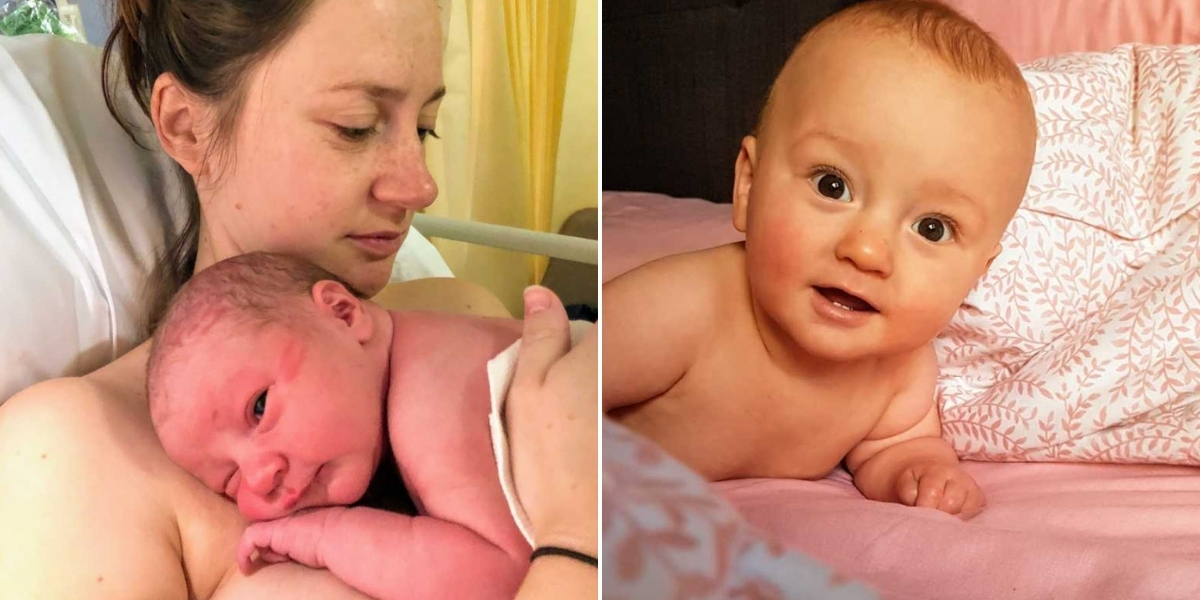
I didn’t have a birth plan. I was certain I didn’t want to set my heart on laboring in a specific way, only to be disappointed if things didn’t go according to plan. I knew that would only make the experience more stressful. The only thing I felt unwavering about was breastfeeding. I had devoured books, scoured online articles, and bombarded family and friends with questions. I felt confident it would come naturally, and I was genuinely excited to nurture my baby that way. When we arrived at the labor ward, I told the midwives I wanted skin-to-skin contact immediately after birth—the much-lauded “golden hour.” They agreed, but sadly, that’s not how things unfolded.
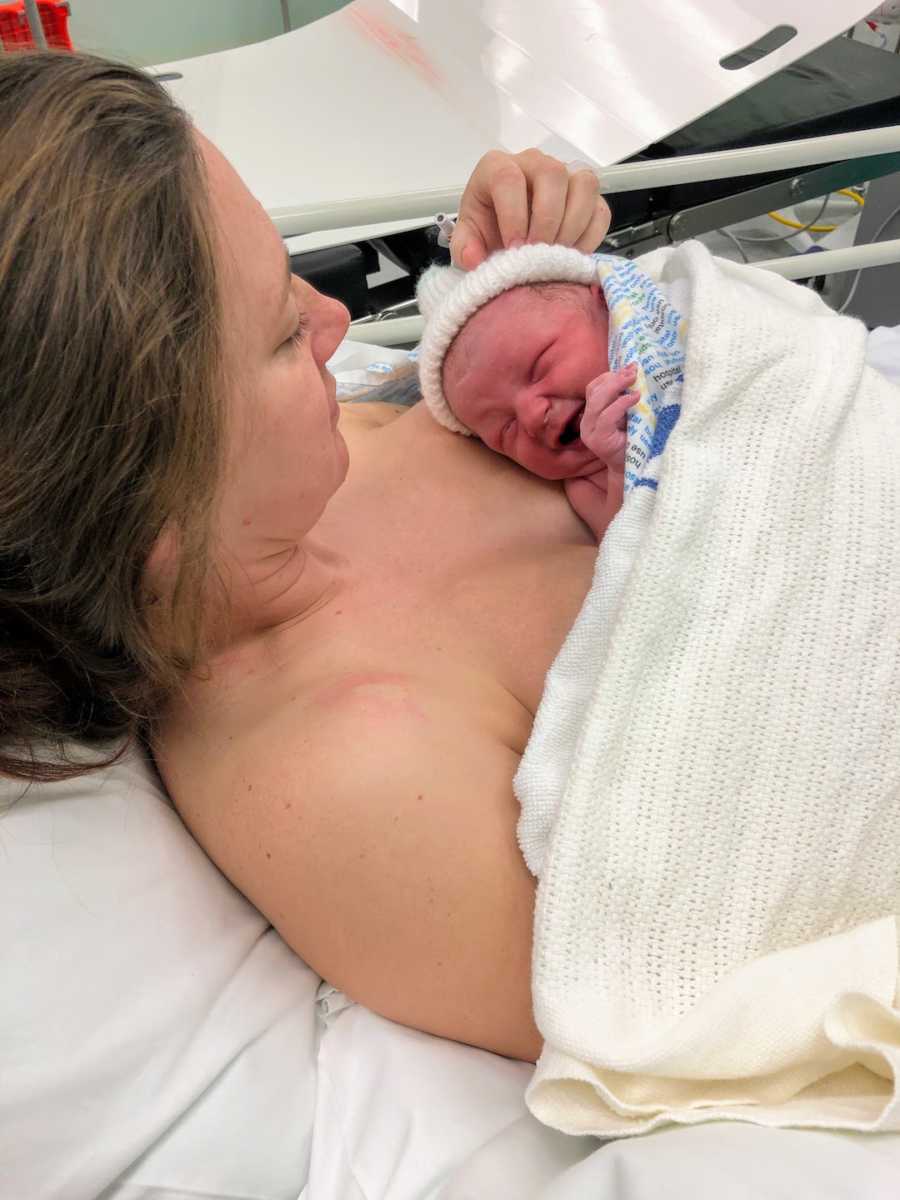
After a very long, slow labor, I ended up needing a cesarean. It wasn’t what we had envisioned, but we wanted our baby delivered safely. At 4:37 a.m. on December 2, 42 hours after my water broke, George Brodie Shooter entered the world with a healthy cry. Relief washed over us. But as the surgeons continued their work, Brodie was whisked away to be weighed, and I didn’t actually see him for seven minutes. James, my partner, went to check on him while I stared at the clock, feeling time crawl. When they finally brought him over, I was still pinned to the table, unable to move my arms. They held him so close my eyes couldn’t focus; he was just a fuzzy, blanket-wrapped shape in my peripheral vision.

This wasn’t the golden hour I’d anticipated. That crucial hour, often highlighted in breastfeeding literature, had slipped past us. About an hour later, we were on the ward. I was still numb from the spinal anesthesia and utterly exhausted, but eager to meet my son properly. At the first opportunity, a nurse placed him on my chest, and we attempted the first feed. She helped position him for a correct latch and left us to it. I expected some discomfort at first, but felt nothing. Elated, I thought, “Well, this is easy!” I was overjoyed that at least this part seemed to be going right.
For the next few feeds, everything seemed fine, but soon tiny twinges began. Within two days, every latch sent stabbing pain through my chest. The pain was unbearable; I screamed into a pillow or bit my fist each time James lifted Brodie onto me. Nurses tried to help, but each gave different guidance. One explained the spinal tap had likely gone too high, numbing my sensations initially, so I hadn’t established a comfortable position or proper latch. Meanwhile, Brodie had been gnawing on me for nearly 24 hours, and now I could feel every bit of it.

It became clear my nipples were blistered and bleeding, but I was desperate to feed him breast milk. Formula simply wasn’t an option in my mind. I convinced myself all new moms must struggle this way. Over the next week, feeding remained agonizing. Fifteen-minute sessions left me exhausted, and Brodie wasn’t getting the fattier milk at the end of feeds. Hungry and frustrated, he suckled ferociously, chewing on my nipples with his gums and the hard palate of his mouth. It felt like feeding a tiny piranha.

Labor pains from days earlier seemed mild compared to this. At least my cesarean wound barely registered. Despite repeated pleas for help, midwives and health visitors simply advised me to “persevere.” They observed feeds, acknowledged the problem, and suggested painkillers and nipple cream, but nothing changed. Brodie’s frequent feeds prevented healing. Expressing milk into a cup only caused him gas, and pumping was discouraged for fear of confusing his latch. As a result, Brodie’s weight dropped to 12% below birth weight, finally prompting the health visitor to step in—but her advice, to feed more often and longer, brought me to tears. She increased visits to monitor him, but she couldn’t grasp how much pain I was in or how little milk he was taking.

Guilt for not satisfying my hungry baby weighed heavily. One night, in the early hours, all three of us cried. I couldn’t endure another feed, and James was helpless, cradling Brodie and trying to soothe him. We lived in a remote part of the Scottish Highlands, with no shops open overnight, and no formula in the house. The pressure was crushing.

That night, I reached my breaking point. I grabbed the breast pump we had been advised to avoid until six weeks in and turned it on. Though still painful, pumping was far more manageable than direct feeds. Within moments, I had enough milk for Brodie’s feed. The house, usually filled with his desperate cries, became quiet except for the gentle sound of sucking. He fed eagerly, fully satisfied, and finally slept for hours. Watching him content and nourished was a relief beyond words.
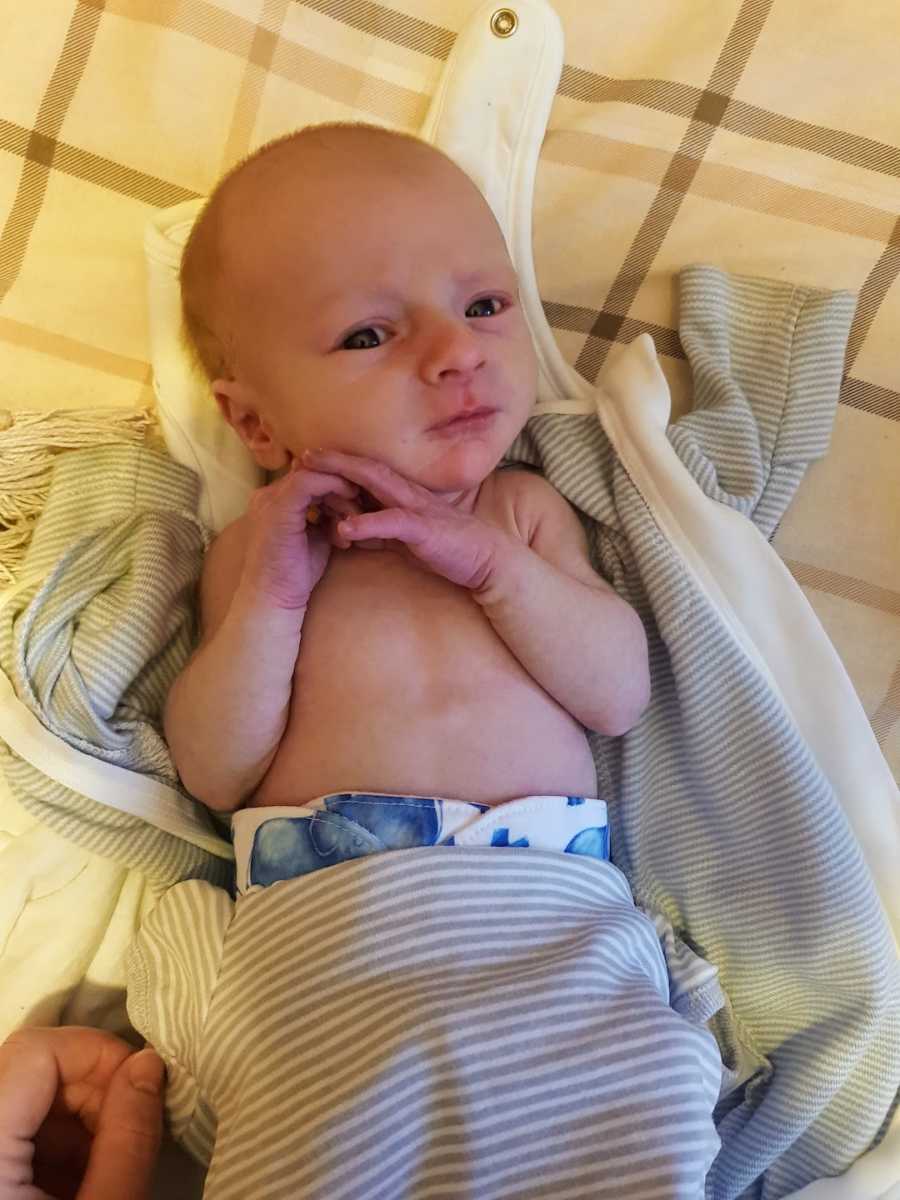
From that night on, James and I alternated between pumping and direct feeds. The next day, the combination method seemed to work beautifully. Brodie accepted both the bottle and breastfeeding, and I was able to rest and heal. While our health visitor remained cautious, advising we gradually reduce pumping, it was impossible to argue with the progress we were seeing. My healing and Brodie’s comfort confirmed we had found our rhythm.


Over the following weeks, the latch remained imperfect, but breastfeeding became far more enjoyable. We gave him a bottle before bed for a settled night, and sleep improved for all of us. Pumping remained demanding—every two hours, often taking longer than a feed—but James’s support and our routine made it manageable. Living far from family added challenges, but we coped. I also discovered, through research, that breast milk could be donated to milk banks for premature or ill babies—a lifeline for both them and anxious parents like me.

Fortunately, my supply flourished. I produced more milk than Brodie could consume, and we stored the excess, which eventually allowed us to donate over 12 liters to Milk Bank Scotland. Brodie never missed a drop, and formula was never needed. Our health visitor, once skeptical, became supportive as his weight and health improved. Seeing his tiny baby fat develop was one of the happiest moments of my life.

Donating milk became incredibly rewarding, helping babies in need and easing some of the guilt I had carried. Breastfeeding is not easy, and many mothers struggle despite the perception that it’s “natural.” I, too, experienced exhaustion, physical pain, and mental strain. Watching a hungry, fragile baby suffer is terrifying. Yet, once we found a method that worked, it was transformative. The closeness, the bond, and the knowledge that we were nourishing him properly made every challenge worthwhile.

Looking back, I realize the first 24 hours with a too-effective spinal tap, Brodie’s early feeding habits, and inconsistent advice set the stage for our struggle. But with persistence, creative problem-solving, and support, we overcame it. My main advice for new mothers: insist on a breastfeeding specialist from the start, trust your instincts, and remember that every baby is unique. Donating milk, too, is a profoundly rewarding option if you can—it helped me feel proud of my body and know we were supporting the most vulnerable babies.

Writing this, over a year later, it all still feels fresh. Despite the lows, we are blessed with a happy, healthy son, and I wouldn’t change a moment of our journey. Now that I’ve returned to work, I’ve reduced pumping, but I hope to breastfeed again in the future and continue donating whatever I can. Our journey wasn’t easy, but it made us stronger as a family and gave us a profound appreciation for the power and beauty of breast milk—it truly is liquid gold.