Balance is defined as the ability to stay steady or stable to avoid falling. It’s an elusive concept, one that people everywhere struggle to find—and I’m no exception. Over the years, I’ve worn many hats: wife, mother, teacher, blogger, and volunteer. I’ve spent much of my adulthood trying to juggle these roles in a way that feels fair to everyone while keeping my own head above water. Sometimes, I’ve failed spectacularly.

These roles alone can be overwhelming, but there’s another role I never chose: I’ve spent the last 38 years as a chronic illness patient—24 hours a day, seven days a week, all year long. Living with four autoimmune diseases has been a journey of constant challenge, but it’s also been a teacher, offering lessons in resilience, courage, and self-compassion.
I was that little girl screaming in the doctor’s office, crouched under a chair and hoping the nurse couldn’t reach me with her enormous needle. Often, the tears began even before we arrived, as my mother’s gentle voice tried to coax bravery from me. I tried to hold back my fear, but usually my screams shattered the calm of the room. By age twelve, I could suppress the crying, but the fear still clung to me. Shots were my greatest nemesis—except maybe for the school bully who mocked my buck teeth daily.
One day, our reading teacher assigned a 20-minute presentation. At twelve, it seemed overwhelming, but preparing it was fun. On presentation day, I remember a classmate named Tommy explaining a disease he had: diabetes. He demonstrated using an orange to show how he injected insulin every day to survive. I was captivated by his bravery. That night, I prayed in my room, a nightly plea: “Please God, if I ever have to have a disease, don’t let it be that one.”
Three years later, after months of extreme fatigue, rapid weight loss, unquenchable thirst, and frequent trips to the bathroom, my prayers were answered differently than I expected. I was diagnosed with type 1 diabetes, my first autoimmune disease. My immune system had attacked my pancreas, stopping insulin production. I cried throughout my hospital stay, overwhelmed and shocked by this new reality. When I left, I had conquered my fear of syringes, and my blood sugar was partially stabilized. The courage I discovered in those early days became the foundation for living with this lifelong condition.
Managing diabetes at that time meant multiple insulin injections daily and finger sticks five or six times a day to monitor blood sugar. Nurses drilled into me the frightening long-term consequences: blindness, nerve damage, heart disease, amputations. Though I occasionally longed to break free from constant monitoring, the risks kept me diligent. College years tested me in new ways: handling my disease alone, juggling stress and dietary changes, and learning to survive without my family’s constant support. Somehow, I made it through, driven by the hope of one day being healthy enough to have children.

Today, technology has made life with diabetes more manageable. I use an insulin pump, which acts like an electronic pancreas, delivering insulin continuously, and a continuous glucose sensor that communicates with the pump for better control. Every day, I apply math I never thought I’d use again—counting carbs, calculating boluses, adjusting doses—all to stay healthy.
Even with technology, diabetes requires constant vigilance. I wake early to refill my pump and change infusion sites, and I stay up late charging sensors and checking blood sugar. Alarms sound in the night, warning me of highs and lows. Minor mishaps—a ripped pump tube, a misdirected insertion, a sudden stream of blood—can throw off the day. Managing diabetes is relentless, time-consuming, and affects every hour of every day, no matter how strong or determined I feel.
Fifteen years after my initial diagnosis, I began feeling awful again. My husband, Paul, and I were raising three toddlers, and I could barely function. I suffered from stomach pain, nausea, diarrhea, and profound weakness. My doctor told me I looked perfectly healthy—just a tired mom. I insisted, “I am tired, yes, but this is beyond normal. I could keep up with my children before, and now I can’t even move from the couch.” Paul stepped in multiple times a day to help me. Without his support, we couldn’t have managed.

Eventually, after visiting multiple doctors and enduring many tests, I received my second autoimmune diagnosis: celiac disease. Gluten triggered my immune system to attack the villi in my small intestine, making nutrient absorption impossible. Management was simpler than diabetes but life-changing. I eliminated gluten from my diet entirely—back then, gluten-free foods were scarce—and slowly my body healed. Still, navigating hidden gluten in dressings, sauces, cosmetics, and even envelope glue required constant vigilance. I grieved for the limitations this disease imposed, even while knowing my situation could have been far worse.

My third autoimmune disease arrived gradually. I ignored early symptoms as I focused on family and career: severe headaches, erratic menstrual cycles, and temperature swings. Brain fog clouded my thinking, and sometimes my fingers wouldn’t obey my brain’s commands. My right leg often went numb for days, lips tingled, and my eye felt like it was crawling. Pain struck both thighs simultaneously, making it impossible to stand. Exhaustion became my constant companion, and even breathing felt like work. Misdiagnoses came—pneumonia, rashes, heart palpitations—but no answers.
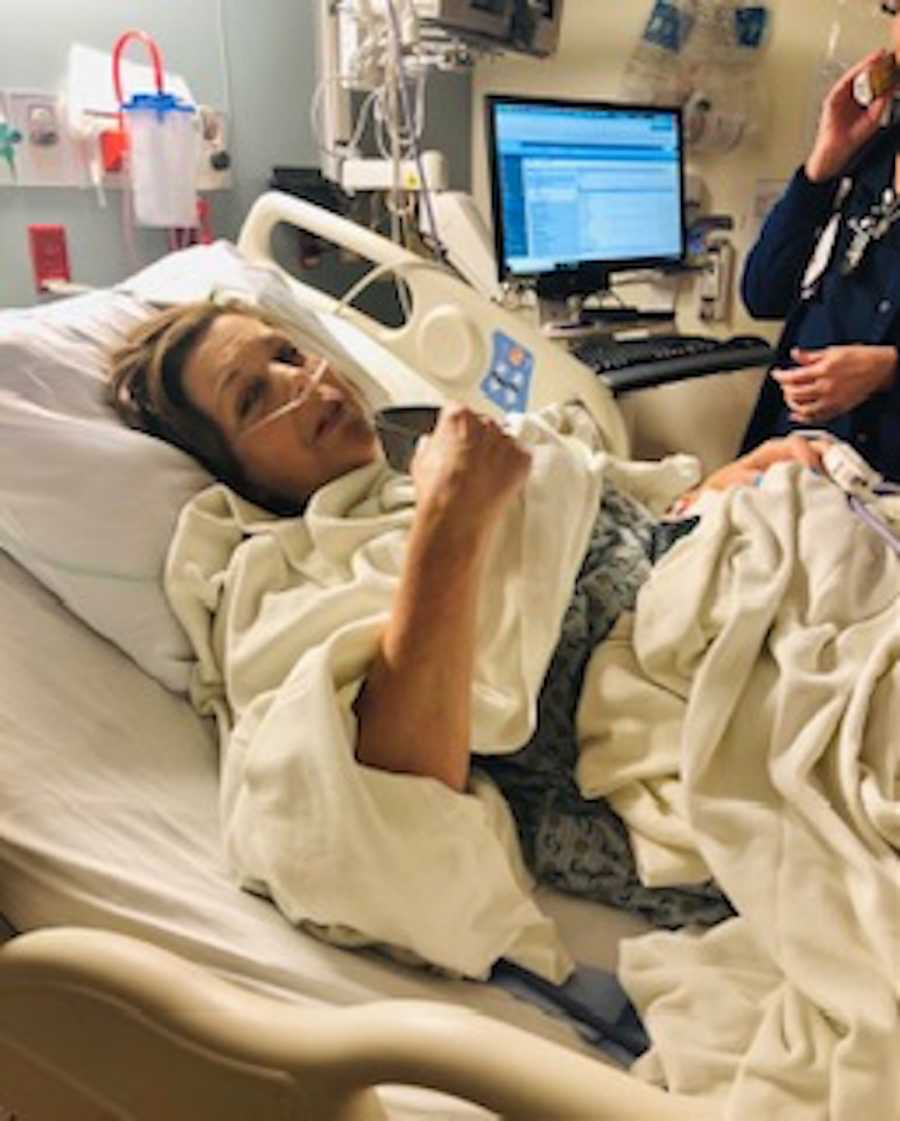
My primary care doctor persisted. Tests revealed lesions across my spine, liver, spleen, and lungs. A spleen biopsy led to a diagnosis of sarcoidosis, a multi-system inflammatory disease. While many patients recover, about 30%—including me—require ongoing immunosuppressant therapy. Five years later, after treatments and frequent visits to Cleveland Clinic specialists, I am learning to accept that this will be a lifelong challenge.

Amid this, I received a fourth diagnosis: Hashimoto’s disease. Daily medication helps, but my hormone levels are still off. I am learning to navigate this condition while balancing the others.
Living with chronic illness demands courage, strength, and stamina. Many autoimmune diseases are invisible, leaving patients appearing healthy while quietly battling daily struggles. Each diagnosis brings grief—sometimes brief, sometimes long—but acceptance eventually comes. Adapting to a “new normal” and practicing self-kindness are essential.
After 38 years, I’ve discovered that taking care of myself is the foundation for managing everything else. I’ve learned this the hard way—like the time I passed out from low blood sugar while trying to juggle preparations for out-of-town guests. Paul had to call 911 as dinner burned. I realized: I cannot care for others if I neglect my own health.

I’ve learned to prioritize wisely, whether in my career or personal life. Stress, caffeine, and poor health choices once caused preventable consequences. With experience, I now make smarter decisions, keeping life and work manageable.

Family remains my heart’s center. For years, guilt nagged me over missed events or moments spent grading papers instead of playing games with my children. But my kids grew into compassionate, empathetic adults. Their understanding, combined with the love we shared, taught me that I had been doing the most important thing all along—showing unconditional love. I no longer let guilt overshadow my care for myself.

Balance also means pursuing goals. Everyone climbs their own mountain, and progress—no matter how slow—is still progress. I am proud of my master’s degree, my awards, completing a 5K despite finishing last, and launching a blog to help others with chronic illness. I work when I am able, rest when I need to, and set my own pace.

Balance, I’ve learned, means knowing what truly matters and putting my health first. When I do, everyone benefits. With understanding, persistence, and love, we all win.