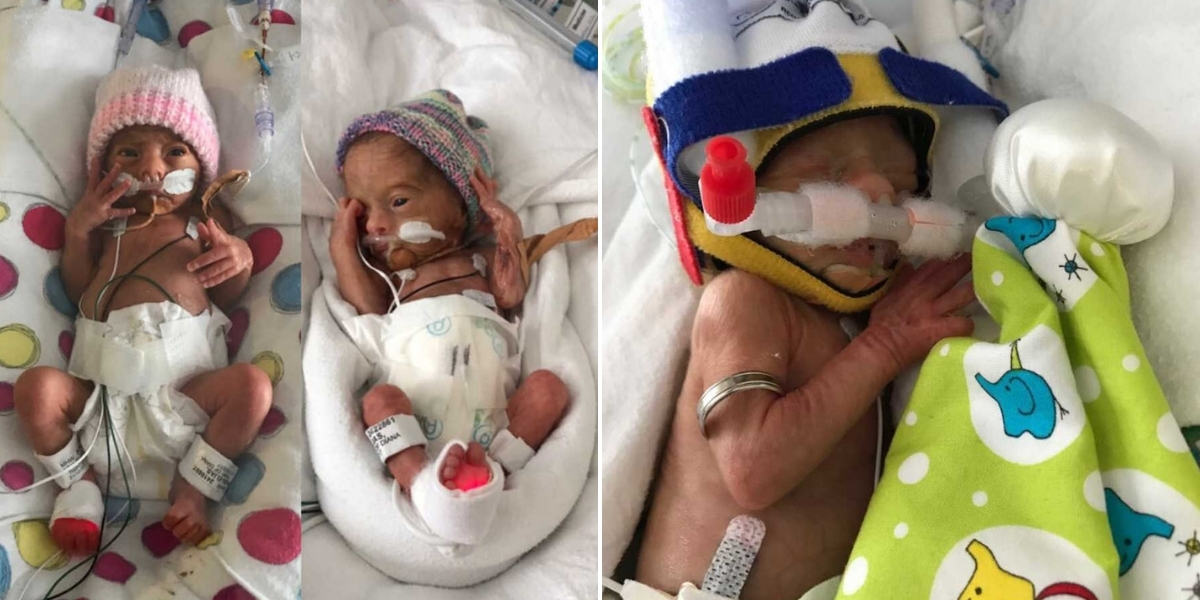
“It takes a village to heal a mother.”
This is the truth I learned not long after I began to recover from the trauma of my pregnancy, the birth of my identical twin girls, and our long, uncertain days in the Neonatal Intensive Care Unit (NICU) and Special Care Nursery (SCN).
My daughters were born prematurely on 21st October 2017, and it wasn’t until almost two years later that I truly began to feel like myself again. My recovery was fueled not only by my love of running and writing my book 30 Weeks 1 Day, but also by the incredible network of people who walked with me through every challenge along the way.
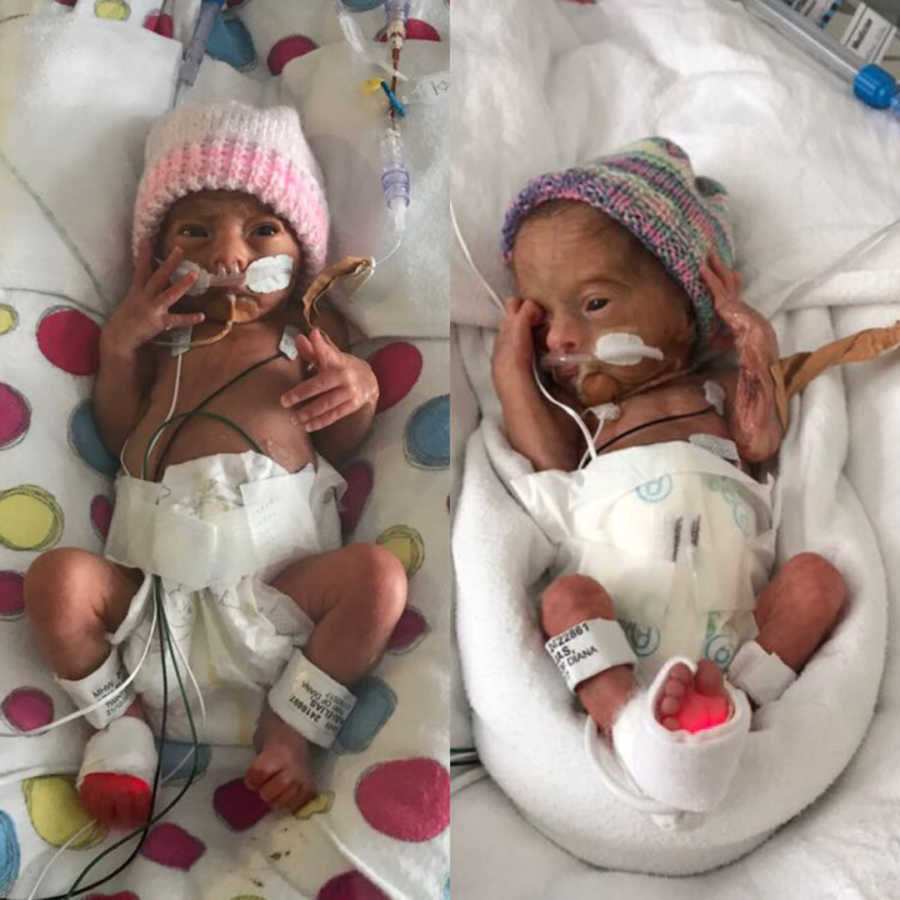
My story begins even before my daughters existed, back in December 2015, when I was diagnosed with endometriosis. For years, I had struggled with infertility without understanding why. Receiving the diagnosis was a shock. I felt as though I had failed my body somehow, believing I should have been able to prevent this. But I would later learn that endometriosis is out of anyone’s control, even though I had experienced symptoms since my early teenage years.
I had consulted doctors before about the severe pain I endured, yet remained undiagnosed. I had begun to accept that this was just the norm for women with periods. Endometriosis affects everyone differently, but for me, it caused infertility and a constellation of exhausting, often debilitating symptoms: sharp abdominal pains and cramps, brain fog, headaches, heavy bleeding, fatigue, mood swings, anxiety, and depression.
After two surgeries to manage the condition, by April 2017, I finally fell pregnant. It was a moment for celebration, yet tinged with apprehension. I couldn’t help but worry that something could go wrong, given the long, difficult journey I had endured to reach this point. Pregnancy eased some of my endometriosis symptoms, but even three years later, it remains a condition I manage daily.
Relief washed over me when I saw that positive pregnancy test. I realized, finally, that my body could conceive. That relief was followed by cautious excitement—and then by a subtle, nagging anxiety. At first, we believed there was only one baby.
It wasn’t until around ten weeks that we discovered I was carrying twins. One morning, after experiencing bleeding, I called my obstetrician, who urged me to come in immediately for an ultrasound. I was terrified as I lay on the bed, unable to look at the screen. Instead, I watched my obstetrician, trying to read her expression.

Then she said words I will never forget:
“You should take a look at this. It’s twins! And I think they are identical.”
I didn’t yet grasp the risks that came with identical twins sharing a single placenta. I was oblivious to the challenges that lay ahead, focused only on the hope that my babies would be okay.
In the early weeks, my pregnancy seemed manageable. Yet I had only one placenta instead of two—a red flag for identical twins, who sometimes face unequal blood distribution. At 16 weeks, I was diagnosed with twin-to-twin transfusion syndrome (TTTS), a rare and potentially fatal condition where one twin donates blood to the other, leaving one undernourished and the other at risk of heart failure.
I was immediately placed under the care of the Mercy Perinatal team at the Mercy Hospital for Women in Heidelberg. Their expertise would prove crucial over the coming months.
To give my daughters a chance, I underwent surgery to separate the shared arteries in the placenta, using a laser while awake under local anesthesia. Without this intervention, their survival chances were only 10%. The procedure succeeded, but complications continued: Twin One needed two lifesaving blood transfusions, also performed while I was awake. I had prepared mentally for the laser surgery, but the transfusions left me nearly broken. Yet my decision to continue the pregnancy meant enduring every challenge necessary to save them.
Over the next months, the perinatal team monitored me tirelessly. I underwent 52 ultrasounds, three major procedures, endless blood tests, MRIs, and regular fetal monitoring, all punctuated by constant anxiety. Finally, at 30 Weeks and 1 Day, my girls were born. Holding my breath, I prayed they would too.
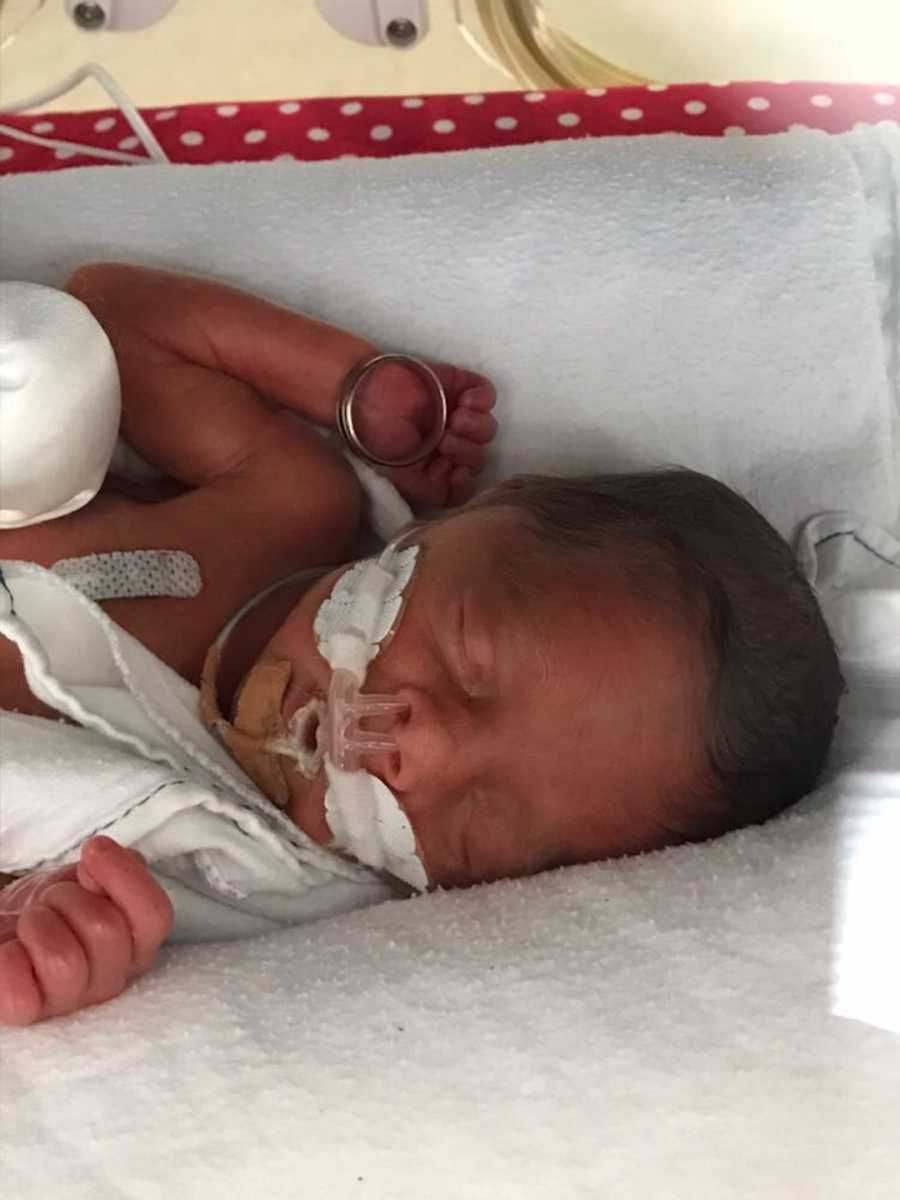
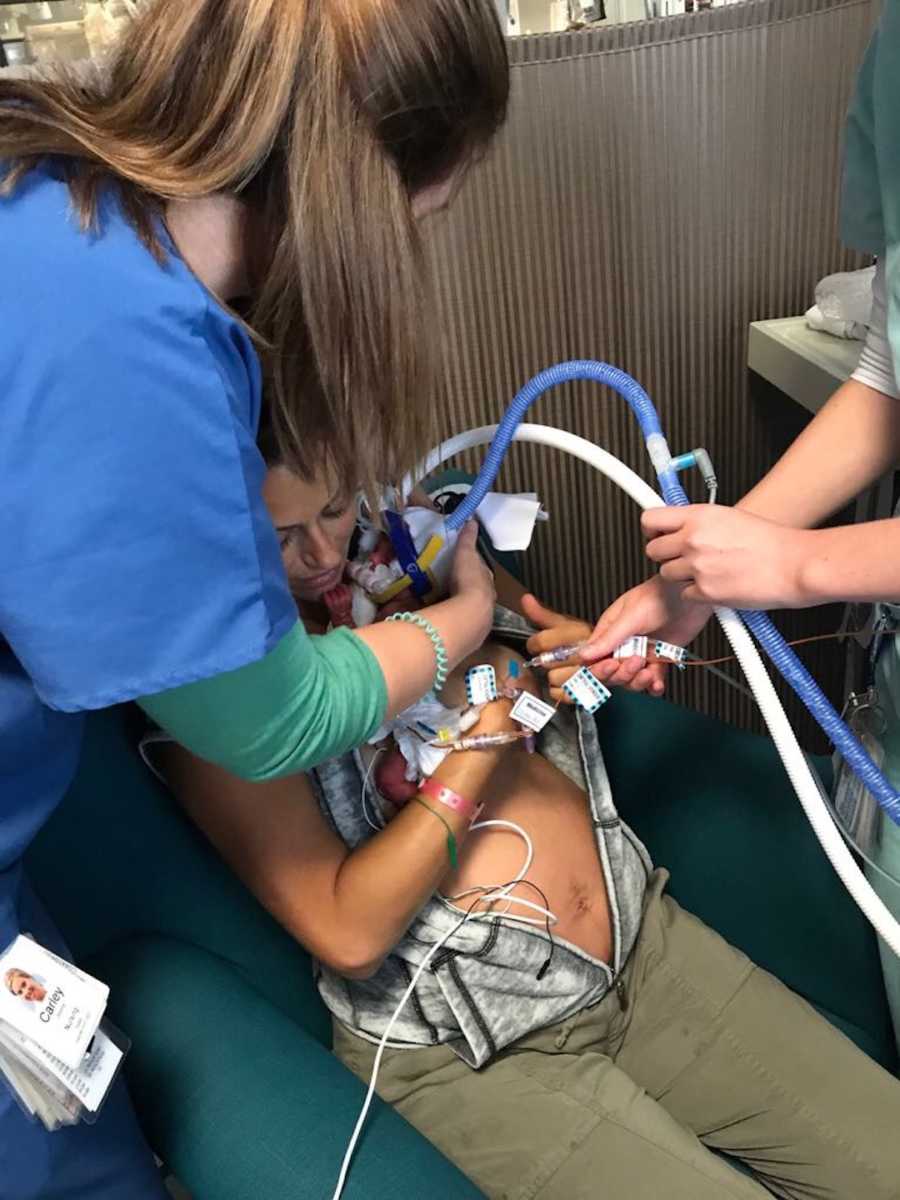
The birth marked the start of a new, harrowing phase. My babies were immediately admitted to NICU and SCN, and we faced months of uncertainty. Each day in utero had been a miracle, but now we counted days in hospital, hoping for health, growth, and strength.
My husband Cam and I spent almost an entire season in NICU and SCN. Adrian’s early complications resolved relatively quickly, but Evie developed necrotizing enterocolitis (NEC) at just four weeks old—a potentially fatal infection that required urgent treatment. Adrian came home three weeks before Evie. Even after recovery, Evie needed oxygen and later surgery for two hernias. It wasn’t until around six months of age that she began to thrive and show her true personality.
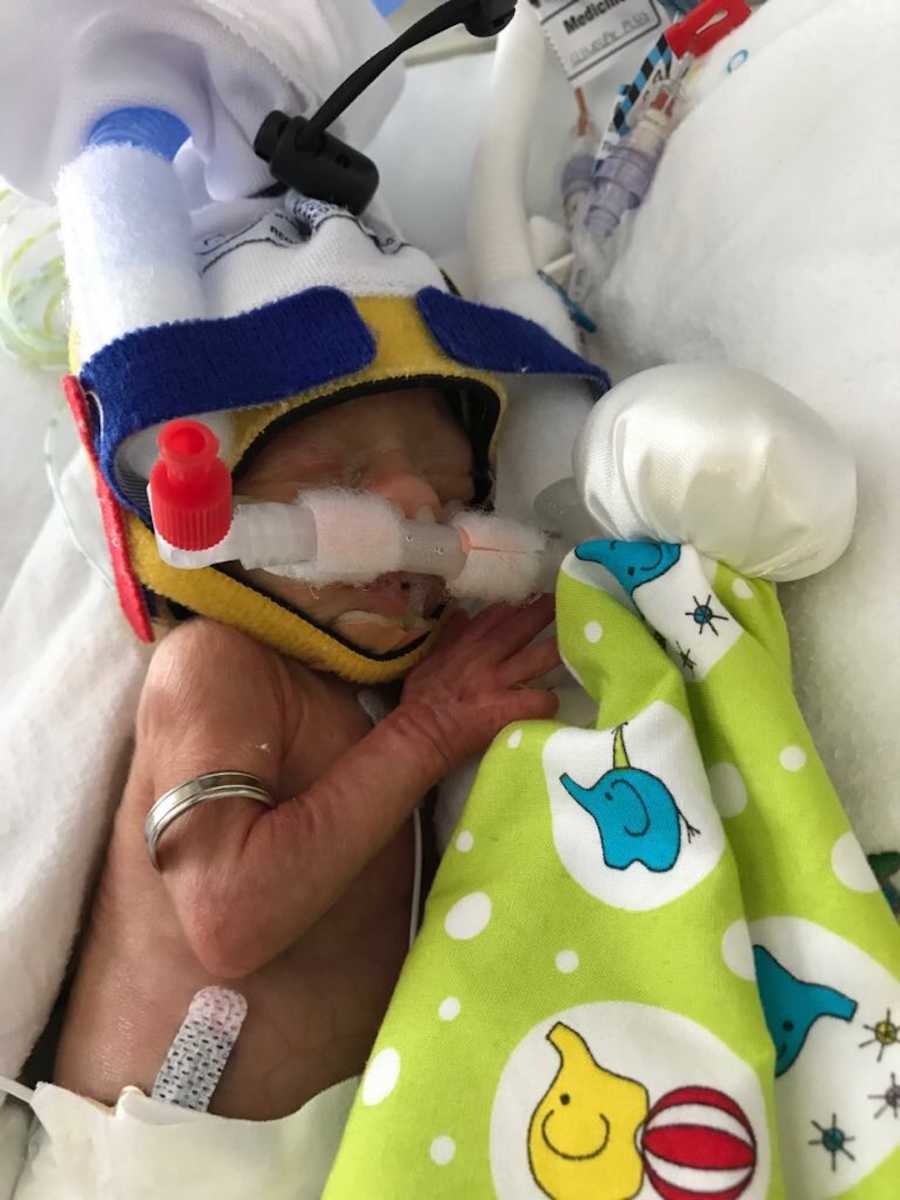
By the time both girls were home, I was emotionally shattered. I had feared losing them every day of pregnancy and NICU life. I experienced postnatal depression, anxiety, and trauma—reactions that, in hindsight, were natural and justified.
Recognizing I needed help, I sought professional support. Almost three years later, I continue to see my psychiatrist. Therapy helped me navigate not only the trauma of pregnancy and NICU but also the transition into motherhood and the restoration of my confidence. Seeking help was daunting, yet it became a cornerstone of my recovery.

They say it takes a village to raise a child. I believe it also takes a village to heal a mother. Writing 30 Weeks 1 Day connected me with incredible people who nurtured my healing simply by engaging with my story. Sharing experiences of difficult pregnancies, anxiety, postnatal depression, and PTSD is vital—not just for others, but for our own recovery.
I wrote initially for my sanity, when running was no longer safe during pregnancy. Later, writing became my therapy, helping me work through postnatal depression and anxiety. It gave me peace and became a lifeline I didn’t fully realize I needed.


Through all the fear, procedures, and sleepless nights, I emerged with gratitude—for my daughters, my husband, the medical teams, and the many small acts of support that helped me heal. In the end, the village that raised my children also healed me, one story, one conversation, and one step at a time.