“She has to be exaggerating.
She isn’t actually sick.
She must be dramatic.”
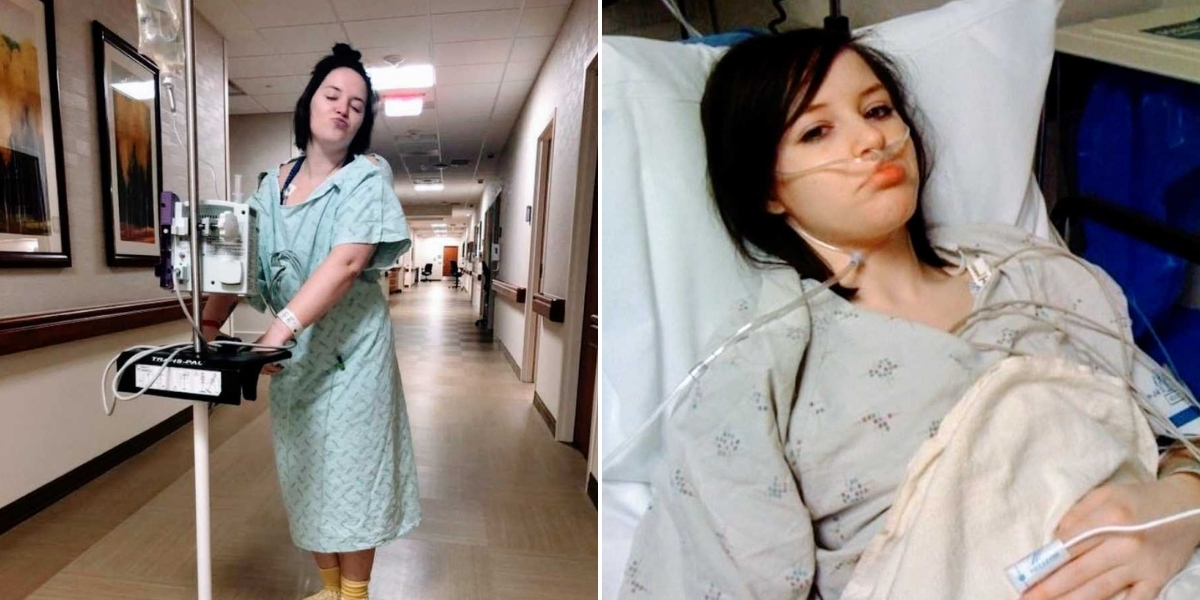
These are the thoughts racing through my mind as I’m rushed into the Emergency Room, trying desperately to stay calm. I find myself repeating the same sentences over and over: “I’m not an addict. I’m not an alcoholic.” It’s a conversation I had far too many times—constantly begging doctors to take me seriously, to see that I was truly sick. Being dismissed, written off, or misunderstood by the very people meant to help you is something that haunts me to this day.

But my story doesn’t begin here. It actually starts long before the diagnosis. I never had the typical stomach issues associated with Celiac Disease. On the outside, I was the picture of health: an all-star cheerleader, active, full of life, seemingly invincible. No one would have guessed the struggles that were silently building inside me.
I was 17 when I experienced my first attack of Pancreatitis. After a week in the hospital, I was discharged with a simple explanation: it was a “fluke thing,” and as a precaution, I should follow a low-fat diet for a few months to give my pancreas a rest. No one thought to test me for Celiac Disease, no one considered that something more serious might be wrong. I tried to return to my normal life while sticking to the low-fat diet, but something had shifted inside me. Stomach pains were constant. My hair was falling out. Bruises appeared without reason. I weighed barely 90 pounds, and my body felt like a prison. I suffered through eight consecutive sinus infections, injuries that refused to heal, and a constant sense of exhaustion that no amount of rest could fix.
Less than five months later, it happened again. The pain was unbearable—sudden, searing, and overwhelming. One moment I was okay, the next I was blacked out on the floor, writhing, being assessed by paramedics. Another attack of Pancreatitis. During this hospital stay, a Pediatric Gastroenterologist came to see me. He barely glanced at my chart, looked me over, and said, “Sweetheart, you don’t look so good. We need to figure this out.”
After only ten minutes of questions and observation, he suggested what no one had mentioned before: Celiac Disease. Panic washed over me—I had no idea what that meant. Back then, Celiac wasn’t widely talked about. But we didn’t wait. An endoscopy was performed, and the results were shocking. A healthy esophagus has villi—small finger-like projections that absorb nutrients—lined in light pink. Mine were gone. The lining of my intestines was dark purple, burned-looking, severely damaged. Blood work confirmed the worst: my body was attacking itself. My Celiac genes had been triggered without my knowledge, and I had been consuming gluten for months, unknowingly fueling the damage.
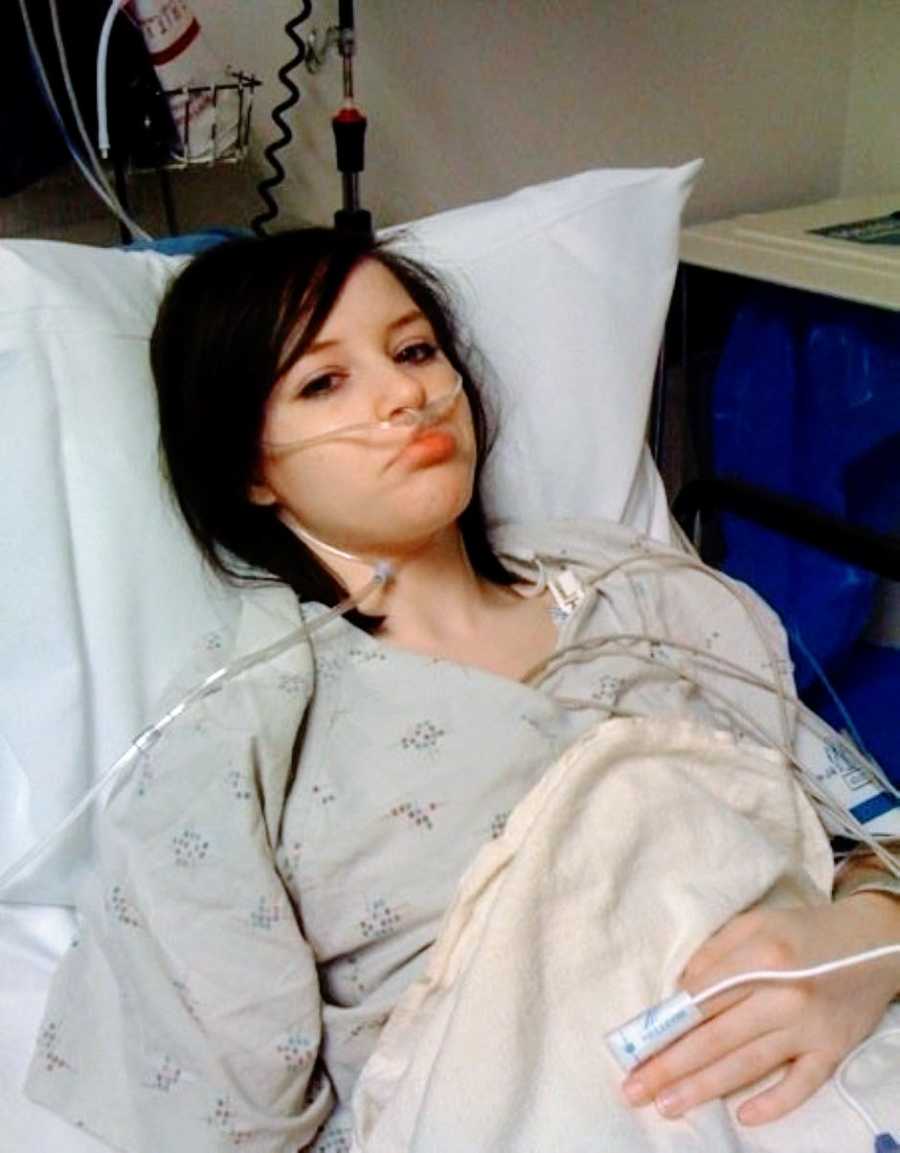
The doctor reassured us: “You will have a new life. A healthier life.” I believed him—but the reality of living gluten-free was more complicated than I imagined. Gluten was everywhere: in foods, toiletries, makeup, even glue. And it came under countless names—barley, rye, oats, wheat protein, malt. Reading labels became a daily ritual, often discouraging, and eating out felt like a dangerous game of Russian Roulette. One crumb of gluten could send me back to the hospital. Cross-contamination was my enemy.

Eleven years ago, gluten-free options were scarce and often unappetizing. Today, grocery stores offer an abundance of tasty alternatives, and for that I am truly grateful.
A few years into my journey, after strictly following a gluten-free lifestyle, new stomach problems emerged. My doctors had assured me I’d be fine—but my body had endured years of inflammation before diagnosis. The damage had caused Cholecystitis, a blockage in bile flow from my liver to my duodenum, requiring gallbladder removal. I thought this was a minor setback, but it was only the beginning.
Persistent pain led to more ER visits, more tests, and finally the realization that scar tissue in my pancreas had developed from prior inflammation, blocking the pancreatic ducts. I underwent a Sphincter of Oddi procedure, which was successful—but it triggered another full-blown pancreatitis attack. Lying in a hospital bed for twelve days, I wondered if this was my life forever. Could I ever be truly healthy? By then, it had been four years since my initial Celiac diagnosis.
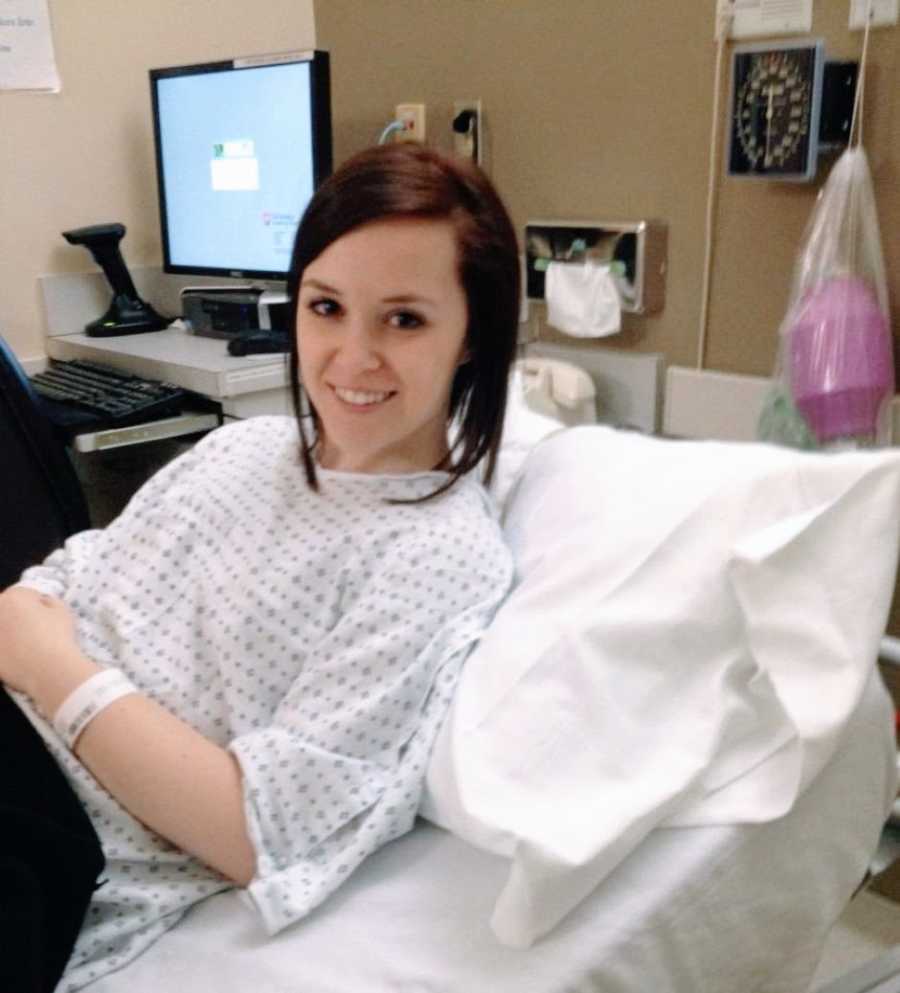
Slowly, life began to turn around. I learned to navigate the realities of Celiac Disease: reading labels, discovering new recipes, avoiding cross-contamination, and redefining what “normal” eating looked like. Dating was a challenge—explaining why I couldn’t eat at certain restaurants or be kissed after a meal was awkward and often embarrassing. I eventually stopped trying to make others understand. This wasn’t a fad or a choice; gluten could put me in the hospital for weeks.
Over the next seven years, I adapted. But unknown stomach pains and nausea continued. ER visits were still common. I was diagnosed with Chronic Pancreatitis, ulcers, and gastritis—all consequences of years spent undiagnosed and untreated for Celiac Disease.

Eleven years post-diagnosis, my lifestyle has transformed. I no longer eat out to avoid cross-contamination and have eliminated most processed foods. Clean eating isn’t dull; it’s an adventure filled with new recipes and discoveries. After over a decade, I finally feel what true health is like. It has taken years to reverse the damage, and I wish more people understood that Celiac Disease isn’t just a “food allergy.”
Today, I use social media to raise awareness, showing people that gluten-free meals can be delicious. Self-care—physical and emotional—is essential. It’s okay to rest, to feel frustrated or sad. I’ve learned that I don’t need others to understand my disease. Each person’s journey with Celiac is unique.

My path hasn’t been easy, but it has shaped who I am today: a well-adjusted, healthy adult, far too obsessed with her dog, but otherwise thriving. Sharing my story is my way of helping others navigate this disease, offering hope and solidarity to those who may feel alone.